NARRATIVE/SYSTEMATIC REVIEWS/META-ANALYSIS
Why Blockchain Benefits Don’t Guarantee Adoption: An Integrated TAM-TOE Analysis of Technology Acceptance and Organizational Readiness
Fatma M. AbdelSalam, DBA, MBA, FACHDM 
Assistant Professor of Population Health Leadership and Analytics, School of Health Professions, University of Texas at Tyler, Tyler, Texas, USA
Keywords: Blockchain technology, digital health transformation, health information systems, healthcare adoption, organizational readiness, perceived risk, technology acceptance model, technology-organization-environment framework
Abstract
Background: Despite blockchain technology’s demonstrated potential to enhance security, transparency, and efficiency in healthcare systems, adoption rates remain significantly lower than predicted, creating a persistent gap between perceived benefits and adoption feasibility. This study addresses the critical question of what explains this adoption paradox by developing and testing a comprehensive theoretical framework that integrates the Technology Acceptance Model (TAM) with the Technology-Organization-Environment (TOE) framework.
Methods: A systematic literature review is conducted following Preferred Reporting Items for Systematic Reviews and Meta-Analyses guidelines to synthesize existing research on blockchain adoption in health care. This study develops four key propositions examining how technology characteristics, organizational factors, external environmental pressures, perceived risks, and system quality collectively influence healthcare organizations’ blockchain adoption intentions.
Results: The analysis reveals that blockchain adoption in health care is influenced by a complex interplay of facilitating and inhibiting factors. Technology characteristics such as perceived usefulness (PU) and ease of use, combined with organizational innovation readiness and technology compatibility, positively influence adoption intention. External factors enhance perceived technology benefits and consequently affect adoption decisions. However, perceived risks moderate the relationship between PU and adoption intention.
Conclusions: Blockchain technology represents a transformative solution for persistent healthcare challenges, but successful adoption requires a holistic approach that simultaneously addresses technology, organizational, and environmental factors. The adoption gap can be bridged through strategic planning that aligns institutional readiness with user incentives, comprehensive risk management, and supportive regulatory frameworks. Future research should focus on establishing ethical governance models to support broad blockchain adoption in health care.
Plain Language Summary
This research paper examines why blockchain technology isn’t being widely adopted in healthcare despite its promising benefits. The study found that adoption depends on three key factors: technology characteristics (usefulness, ease of use, and security), organizational readiness (resources, infrastructure, and leadership support), and external environment (government regulations and market pressure). The research shows that simply having good technology isn’t enough, healthcare organizations need the right resources, training, and support systems in place. Additionally, perceived risks around data security can slow adoption, even though blockchain is designed to be secure. The paper recommends that governments create clear regulations, healthcare organizations invest in infrastructure and staff training, and technology developers build user-friendly solutions. The author concludes that successful blockchain adoption in healthcare requires collaboration between policymakers, healthcare organizations, and technology developers to address technological, organizational, and regulatory challenges simultaneously.
Citation: Blockchain in Healthcare Today 2025, 8: 428.
DOI: https://doi.org/10.30953/bhty.v8.428
Copyright: © 2025 The Authors. This is an open-access article distributed in accordance with the Creative Commons Attribution Non-Commercial (CC BY-NC 4.0) license, which permits others to distribute, adapt, enhance this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See http://creativecommons.org/licenses/by-nc/4.0. The authors of this article own the copyright.
Submitted: July 8, 2025; Accepted: October 18, 2025; Published: December 16, 2025
*Corresponding Author: Fatma M. AbdelSalam, Email: Fatma.abdelsalam@uttyler.edu
Competing interests and funding: The author declares no competing interests.
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
The healthcare industry is under increasing pressure to improve transparency, data privacy, and interoperability. Traditional electronic health record (EHR) systems are often fragmented and vulnerable to data breaches, leading to inefficiencies and compromised patient data.1 The evolution of healthcare technology has been defined by shifts in how data are generated, stored, and shared. From paper-based records to EHRs, the digitization of health care has improved access to information but has introduced new complexities. Health systems often operate in silos, which impedes system interoperability. Data breaches, unauthorized access, and inconsistent patient experiences remain prevalent.2 In this context, blockchain technology offers a paradigm shift. Blockchain technology, recognized for its decentralized, immutable ledger capabilities, has gained significant attention as a potential solution to these persistent issues.3 Initially conceptualized as the infrastructure for Bitcoin, blockchain’s core principles—decentralization, immutability, and transparency—make it well-suited for solving systemic problems in healthcare data management.4
Blockchain technology has emerged as a nascent paradigm for data storage, transfer, and security across various industries. The technology is considered a promising breakthrough that will likely have a significant influence on a myriad of different industries, such as health care, supply chain management, and business.5 The blockchain peer-to-peer network was initially proposed by Satoshi in 2008 and then commercialized in 2009 when Bitcoin emerged as its first use case.6 The healthcare industry has shown interest in exploring the potential of blockchain technology for improving patient care, ensuring data privacy, and streamlining administrative processes.7 Blockchain technology has the potential to transform the healthcare industry by providing a secure, decentralized, and transparent platform for potentially managing patient data, reducing fraud, and enhancing trust among patients, healthcare providers, and other stakeholders.8
Healthcare organizations face dual responsibilities: protecting sensitive patient data and enabling timely access for care delivery and research. Blockchain can facilitate verifiable, secure exchanges of information without relying on a central authority. This has implications not only for clinical data but also for billing, insurance processing, pharmaceutical logistics, and research compliance. As Schiavone and Omrani9 suggest, blockchain is a promising technology that will play a central role in the next wave of digital health transformation. However, the adoption comes with hurdles and challenges. The conservative nature of healthcare systems, compliance demands of the Health Insurance Portability and Accountability Act (HIPAA) and General Data Protection Regulation (GDPR), and high infrastructure costs limit the chance for experimentation. However, governments and enterprises are piloting projects across Asia, Europe, and North America to validate blockchain’s value. This study explores the dynamics for strategies to unlock blockchain’s healthcare potential. Blockchain technology offers a decentralized, secure, and transparent framework that addresses core inefficiencies in the healthcare industry. The increasing need for interoperability, data integrity, and cybersecurity has drawn attention to blockchain’s potential to mitigate challenges inherent to legacy systems.7
Here, it is proposed that blockchain adoption in health care can offer transformative solutions in data sharing, supply chain integrity, patient empowerment, and clinical trial transparency. It highlights emerging use cases and illustrates how blockchain supports trust and accountability. The adoption, however, faces regulatory ambiguity, scalability issues, and resistance from healthcare institutions. Drawing on recent literature,9–12 as healthcare systems strive toward digital resilience, blockchain provides a critical infrastructure layer to secure, integrate, and optimize clinical and administrative operations. In the long term, blockchain could underpin global health data ecosystems that prioritize patient-centric care and cross-border data governance. This study contributes to the ongoing discussion regarding the adoption of blockchain technology in the healthcare industry.
Literature Review
Blockchain technology is a distributed ledger technology that allows transparent and secure transactions without the need for intermediaries.10,13 The technology allows for the creation of a decentralized network of nodes that verify and record transactions in a secure and transparent manner.14 Each transaction is recorded in a block, which is linked to the previous block in a chain, creating an immutable ledger of transactions. This technology has several key features that make it attractive for the healthcare industry, including data immutability, transparency, security, and decentralization.15
The field of health care presents a multitude of opportunities for the implementation of blockchain technology. One of the most intriguing and promising uses of blockchain technology in the healthcare industry is the management of EHRs. The EHR systems that are built on blockchain technology could provide patients with the ability to control access to their health data, improve the confidentiality and safety of health information, and lessen the likelihood of data breaches. The EHR systems based on blockchain technology could also enhance interoperability and data exchange between various healthcare organizations.16,17
The management of the pharmaceutical supply chain is another area that blockchain technology could potentially be utilized to enhance. Blockchain-based systems could improve transparency and traceability in the drug supply chain, thereby reducing the risk of counterfeit drugs and increasing patient safety.18 This would be a significant step forward in the fight against the widespread problem of fake drugs in the healthcare industry.14 Additionally, systems based on blockchain can lessen the administrative burden of managing drug supply networks, which would result in an increase in the healthcare industry’s overall level of productivity.
Synthesis of Literature
Publications on blockchain technology and its applications in the healthcare field are diverse and draw from various streams of literature, including information technology (IT), healthcare administration, and economics, among others. Several studies highlight the technical and regulatory barriers to overcome before blockchain technology can be adopted and deployed in the healthcare industry. For instance, a study conducted by Agbo et al.13 discussed that the primary hindrances to the adoption of blockchain technology in the healthcare industry were the high levels of technological complexity, interoperability issues, and regulatory uncertainty. In addition, the literature highlighted the significance of training, education, and collaboration among stakeholders as means of overcoming these obstacles.
The prospective adoption of blockchain technology in the healthcare industry has been the subject of investigation in other studies. For instance, Azaria et al.16 published a study in which they suggested a blockchain-based system for managing EHRs. This system allows patients to control access to their data while also reducing the likelihood of data breaches commonly occurring. The authors placed a strong emphasis on the significance of maintaining data privacy and security throughout the process of adopting and implementing blockchain technology in the healthcare industry. The application of blockchain technology to the management of pharmaceutical supply networks was the subject of research conducted by Kuo et al.19 The authors claimed that blockchain technology improves transparency and traceability in the drug supply chain, thereby lowering the risk of patients receiving fake medications and increasing the safety of patients overall.
The potential economic advantages of using blockchain technology in health care have also been the subject of investigation in several studies. For instance, Abu-Dalhoum et al.20 discovered that blockchain technology can expand the effectiveness of healthcare systems while simultaneously lowering the expenses associated with administrative procedures. The authors highlighted the necessity for healthcare organizations to incorporate a tactical approach to the deployment strategy of blockchain technology. The Healthcare Weekly report4 further substantiates these economic benefits, estimating potential annual savings of $100–$150 billion by 2025 through blockchain adoption in health care, primarily from reduced data breach costs, IT expenses, and fraud.
While the existing literature provides a foundational understanding of blockchain’s potential in health care, a more critical analysis reveals certain limitations and areas for deeper exploration. Many studies, while highlighting the benefits, often remain at a conceptual level or focus on technical aspects without sufficiently addressing the complex organizational and environmental factors influencing adoption.9 For instance, early reviews tend to summarize findings without delving into the methodologies, limitations, or conflicting results of cited works.21 This paper aims to bridge this gap by integrating recent empirical findings and addressing the practical barriers to adoption.
Recent research, such as Bazel et al.,3 emphasizes that despite the transformative potential, blockchain adoption in hospitals remains minimal due to high implementation costs, lack of standardization, and resistance to change. Mutambik et al.22 further identified administrative challenges, usability issues, and regulatory frameworks as significant barriers from the perspective of healthcare professionals. These studies highlight the need to move beyond theoretical discussions and focus on actionable strategies to overcome the real-world impediments.
Furthermore, while interoperability is frequently cited as a key blockchain benefit, the challenges in achieving it with existing legacy systems are often underestimated. Kasyapa and Vanmathi 2 provide a comprehensive investigation into these issues, highlighting the complexities of integrating blockchain with diverse healthcare IT infrastructures, such as database incompatibilities and network infrastructure limitations. Similarly, the financial implications, while often framed in terms of potential savings, also present significant upfront investment barriers that require more detailed analysis and justification.4 This article informs future research by emphasizing the need for a holistic approach that considers not only the technological promise of blockchain but also the intricate interplay of organizational, environmental, and human factors that ultimately determine its successful integration into healthcare systems.
Theoretical Framework
Integrated TAM and Technology-Organization-Environment Model
The Technology Acceptance Model (TAM) is a popular theoretical paradigm that investigates how individuals respond and interact with computerized systems, particularly in the context of new technologies. Davis created the model in 1989, and it has since been used extensively to study user behavior and technology adoption.23 TAM consists of two main factors that affect user behavior regarding technology adoption: technology’s perceived usefulness (PU) and perceived ease of use (PEOU).24 The Technology-Organization-Environment (TOE) framework suggests that the adoption of new technology depends on three key factors: the characteristics of the technology, the organization in which the technology is being utilized, and the broader external environment in which the technology is being deployed.25 Many healthcare organizations are in the process of considering artificial intelligence and big data technologies. Therefore, integrating blockchain in their systems will, in turn, expedite the adoption process.10
In the context of blockchain technology in health care, the TOE and TAM can be used to investigate what variables affect healthcare organizations’ openness and adoption of new technologies.25 Hence, to meet the objective of this study, an integrated TAM-TOE framework has been proposed. Compared to the TAM, which analyzes technology adoption at the individual level, the TOE26 framework has been found to be the most robust and widely used adoption model in the technology adoption literature10 and was classified as an organizational-level theory. Integrating the TAM and TOE frameworks provides a more robust theoretical lens, allowing for the simultaneous analysis of individual user attitudes, organizational dynamics, and external environmental pressures.27
As depicted in Figure 1, the proposed integrated model demonstrates how technology characteristics (compatibility, reliability, and facilitating conditions), organizational factors (readiness and innovation readiness), and environmental factors (market pressure, government support, and regulatory environment) collectively influence perceived usefulness and ease of use, ultimately affecting the behavioral intention to adopt blockchain technology and its actual use.28
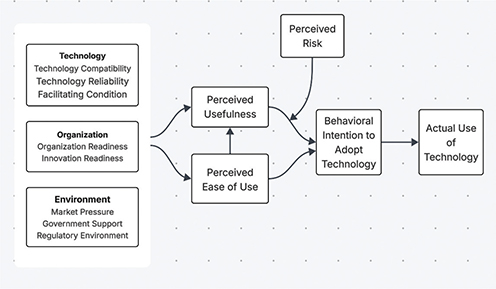
Figure 1. Concept model of factors influencing blockchain technology adoption following the TAM and TOE frameworks. This figure visually represents the integrated TOE-TAM model, showing how technological, organizational, and environmental factors influence PU and PEOU, which, in turn, affect the intention to adopt blockchain technology in health care.28
Methodology
Systematic reviews serve as a foundational methodology within healthcare research, enabling a rigorous synthesis of existing literature to address specific research questions. This approach aggregates findings from previous studies to provide a comprehensive understanding of a topic, as demonstrated by Kuo et al.19 in their examination of blockchain adoption in the healthcare sector. The main objective of this article is to answer the following question:
- What explains the discrepancy between blockchain’s perceived benefits and actual adoption rates in healthcare organizations?
By analyzing both conceptual and empirical research, this review identifies the critical factors that either facilitate or impede the adoption of this technology, thereby consolidating current understanding and highlighting key themes from prior scholarly work. The article selection process for this review was guided by the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) framework to ensure methodological transparency and rigor.
An extensive search was conducted across numerous electronic databases, including Google Scholar, ScienceDirect, Scopus, and PubMed, using a comprehensive search string with keywords such as “TAM-TOE,” ”blockchain,” “healthcare,” “adoption,” and “factors.” All articles that were published between 2014 and 2025 were included. The initial query yielded 740 articles. Following the application of Boolean operators and a backward referencing process, 45 potentially relevant studies were identified. The refinement resulted in a final iteration of 27 peer-reviewed studies deemed directly pertinent to the research for the analysis.
Propositions
Proposition 1: Technology characteristics such as PU and PEOU, along with factors such as innovation readiness and technology compatibility, positively influence the adoption intention of blockchain technology in health care.
Enabling secure, decentralized, and immutable data storage and sharing through blockchain technology could revolutionize the healthcare sector. However, the adoption and implementation of this technology is dependent on various factors, including technology characteristics and organizational factors.29
This proposition aims to explore how technology characteristics, such as legacy system integration, along with organizational factors such as IT staff expertise, training infrastructure, and dedicated innovation budgets, influence the adoption intention of blockchain technology in health care. PU and PEOU are the main factors that affect user behavior regarding technology adoption intention, according to the TAM.25 While PEOU relates to how easily a user perceives a technology to be used and learned, PU refers to how beneficial a user perceives the technology to be in carrying out activities or attaining goals.24 Organizational adoption strategies are important to the successful use of blockchain technology. Healthcare providers and patients are more likely to adopt and utilize blockchain technology if they believe it will improve care delivery and outcomes and will be simple to grasp and use without a lot of practice or training.24
Organizational factors, on the other hand, are related to the context in which technology is being adopted and implemented. The TOE framework identifies three key factors that influence technology adoption and implementation.26 Innovation readiness refers to an organization’s willingness and ability to adopt new technologies, while compatibility refers to the degree to which a new technology fits with existing organizational practices, values, objectives, and norms. The more an organization perceives its technological infrastructure to be compatible, the more capable it is of adopting new technology.30
Kasyapa and Vanmathi2 provide a detailed analysis of these interoperability challenges and propose mitigation strategies. The global pandemic has revealed a lack of interoperability in the current healthcare system and the need for accurate clinical data that can be widely distributed among healthcare providers in an efficient and secure manner.18 The goal of healthcare systems is to eliminate the intermediaries and allow direct and efficient transfer of data and information. Therefore, the proper utilization of blockchain can increase interoperability while maintaining the privacy and security of data.31
In the context of blockchain technology in health care, innovation readiness is a crucial organizational factor that positively influences the adoption of this technology.31 Organizations that are more innovative and willing to adopt new technologies are more likely to adopt blockchain technology.
Research reveals that technology characteristics and organizational aspects play a substantial role in the acceptance and implementation of blockchain technology. The researchers found that PU and PEOU are significant predictors of healthcare professionals’ intention to adopt and use blockchain technology.32
Another study by Mettler33 acknowledged that innovation readiness and technology compatibility are crucial factors influencing the approval and employment of blockchain technology in health care. Building upon the theoretical framework established by Wang et al.10, organizational readiness encompasses three fundamental dimensions: human resource capabilities characterized by IT expertise and technical competencies, financial preparedness evidenced by dedicated budgetary provisions for IT innovation adoption, and technological infrastructure readiness that supports the development and deployment of blockchain applications within organizational contexts.
Proposition 2: External factors such as market pressure and social norms, and government support positively influence the PU and PEOU of blockchain technology in health care and consequently influence the technology adoption intention.
Market pressure is another external factor that can influence the adoption of blockchain technology in health care. However, these same external pressures initially create resistance, workflow disruption, and negative stakeholder reactions that organizations must navigate before realizing positive adoption outcomes. The positive influence on PU and ease of use emerges only after organizations overcome initial implementation challenges, stakeholder resistance, and system integration difficulties. This paradoxical relationship explains why external pressure alone is insufficient for blockchain adoption success; organizations must also develop comprehensive change management strategies to transform initial resistance into eventual acceptance and advocacy. The healthcare industry is becoming increasingly competitive, and healthcare providers are investigating how to improve their services and reduce costs.32
Blockchain technology has the potential to improve the efficiency and security of healthcare operations, which can give healthcare providers a competitive advantage. Moreover, patients are becoming more informed and empowered, and they are demanding better healthcare services. Blockchain technology can improve the quality of healthcare services by providing secure data sharing, reducing medical errors, and enhancing patient outcomes.33 Research has shown that industry competition has a positive impact on IT adoption.34 Zhang et al.35 demonstrated that competitive pressure is a predictive factor for healthcare organizations to adopt health IT. Thus, market pressure can positively influence the adoption and implementation of blockchain technology in health care by creating a demand for more efficient and secure healthcare services.
Early adopters tend to derive considerable competitive advantages. However, early adopters face 50 to 100% higher implementation costs, potentially creating resistance. If healthcare providers observe their peers using blockchain technology in health care and perceive that this technology is highly valued, they are more likely to adopt it themselves.33 Furthermore, if patients perceive that their healthcare providers use blockchain technology to improve their care, they are more likely to accept and use it as well. Thus, social influence can significantly affect the adoption and implementation of blockchain technology in the healthcare field.
Government support is also an external factor that can influence the PU and ease of use of blockchain technology in health care, as suggested by the TOE framework.36 Governments can provide funding and incentives to healthcare organizations to adopt new technologies, including blockchain technology.29 Blockchain technology can enhance the security and privacy of EHRs, which aligns with the goals of the HITECH Act.37 However, a lack of clear government rules and incentives for implementation contributes to the hesitancy of healthcare leaders to adopt this technology.38 Thus, government support can positively influence the adoption of blockchain technology in health care by providing funding and incentives to healthcare providers.
Proposition 3: Perceived risks of blockchain technology negatively influence adoption intention in the healthcare industry through moderating the relationship between PU and adoption intention.
The literature suggested perceived risk as a barrier to the organizational adoption of blockchain technology.36 The perceived risks cause doubt among organizations toward blockchain technology adoption. For example, if technology is perceived as risky with negative personal information disclosure, organizations will be reluctant to adopt it or integrate it into their systems.39 Therefore, it can be proposed that perceived risk can influence the decision of technology adoption.
The perceived risk resulting from using a new technology can moderate the relationship between the technology’s PU and the adoption intention.40 In the context of blockchain technology, trust is particularly relevant, given the technology’s potential to advance the privacy and security of data exchange. Blockchain technology provides a decentralized and immutable ledger of transactions, reducing the need for intermediaries and providing a more transparent and secure way of sharing data.33 In the healthcare industry, trust is significantly important, given the sensitive nature of healthcare data. Therefore, healthcare professionals and organizations must have a high level of trust in any technology used to manage and exchange patient data.14 Nonetheless, the level of trust in blockchain technology significantly influences its acceptance and adoption.
Studies have identified several factors that may affect the level of trust in blockchain technology. These include the lack of technical expertise and knowledge among healthcare professionals, the complexity of the technology, and the need to comply with regulatory requirements.21,31,36,41 If an organization already has the necessary knowledge and skills, they will be more willing to adopt, and if they lack the knowledge and skills, they are less likely.42
Cheikhrouhou et al.1 further emphasize the security enhancements offered by blockchain, which are crucial for building trust in healthcare systems. However, the limited availability of mature blockchain systems within the current market landscape constrains organizational ability to evaluate empirical benefits, thereby fostering institutional uncertainty concerning the value proposition and expected return on investment associated with blockchain technology adoption.41 Healthcare professionals and organizations must be provided with the necessary resources and support to manage the risks effectively and build trust in the technology. Moreover, the acceptance and adoption of blockchain technology in health care must be accompanied by the development of clear standards and regulations that ensure the safe and effective use of technology.19 This requires collaboration between stakeholders in the healthcare industry, such as healthcare professionals, regulatory bodies, and technology providers, to establish common standards and best practices for the use of blockchain technology in the healthcare sector.40
Proposition 4: System quality, such as reliability and security, along with innovation readiness and regulatory environment positively influences the PU and PEOU and the adoption intention of blockchain technology in health care.
The success of a technology implementation largely depends on its system quality, which includes factors such as reliability, compatibility, and security. In the case of blockchain technology in health care, it is crucial for users to have trust in the system’s reliability and security, especially given the sensitive nature of health information.7 In terms of system quality, blockchain technology has several features that enhance its reliability, interoperability, and security.18 For instance, the decentralized nature of the blockchain network makes it less prone to failure. Additionally, the cryptographic algorithms used in blockchain technology provide a high level of security, making it difficult for unauthorized parties to tamper with the information stored on the network.13
The TOE framework proposes that innovation readiness, which encompasses factors such as a company’s ability to adopt new technology and its innovative culture, plays a significant role in the adoption of new technology.43 Innovation readiness can facilitate the adoption and implementation of blockchain technology in health care. Organizations that are innovative and open to emerging technologies are more likely to experiment with and adopt blockchain technology. The more benefits blockchain technology offers to a company, such as security, quick transactions, and immutability, the more likely it is that the organization will embrace innovation.44 In addition, organizations with a strong IT infrastructure and technical support are better equipped to integrate blockchain technology into their existing systems, making it more accessible and easier to use for their employees.29
The regulatory environment is one of the most important external factors that can affect the adoption of blockchain technology in the healthcare industry. The term “regulatory environment” pertains to the policies, initiatives, and incentives that a government implements to encourage enterprises to adopt blockchain technology. As reported in the literature, the regulatory environment plays a significant role in accelerating or impeding the adoption process of the technology and is considered a crucial factor in its adoption.45 Any new technology must adhere to a myriad of regulatory standards since the healthcare sector is heavily regulated.42 For instance, HIPAA in the United States establishes the requirements for safeguarding the confidentiality and security of patient health information. In line with HIPAA regulations, blockchain technology can enhance the security and privacy of health information.37 By ensuring that blockchain technology conforms to regulatory requirements, the regulatory environment can thereby favorably affect the adoption of blockchain technology in health care.10
Based on reports in the literature, the higher the perceptions of regulatory uncertainty, the lower the behavioral intention to adopt blockchain technology.42 Recent reports, such as the International Comparative Legal Guides (ICLG) Digital Health Laws and Regulations Report 2025 USA,46 further emphasize the evolving legal landscape and the need for blockchain solutions to align with these regulatory frameworks. Finally, regulatory support in the form of funding, subsidies, or other incentives can provide a boost to organizations that are considering adopting blockchain technology in health care, making it more financially feasible and less risky.36 Therefore, this proposition suggests that system quality, innovation readiness, and regulatory environment can positively influence the PU and PEOU and consequently the adoption decision of blockchain technology in health care.
Real-World Blockchain Applications
Blockchain technology has moved beyond theoretical discussions and into real-world healthcare applications. One of the most cited examples is MedRec, developed by the Massachusetts Institute of Technology, which enables patients to control their EHRs through a blockchain system built on Ethereum. It tracks access permissions rather than storing medical records directly, thus ensuring compliance and data efficiency. Azaria et al.16 demonstrated how this model promotes patient engagement and accountability. Furthermore, Estonia offers a compelling national-level implementation. The country’s eHealth system uses blockchain to log access to patient data, ensuring transparency and privacy. The integration with national identification systems and government oversight makes Estonia a benchmark in digital health security. PharmaLedger, an EU-funded initiative, is another application that uses blockchain to track pharmaceutical products across the supply chain. This helps combat counterfeit drugs, ensures product authenticity, and improves recall efficiency.47 Blockchain solutions provide end-to-end visibility from manufacturing to patient delivery, enhancing patient safety and regulatory compliance. The technology enhances traceability and enables faster recalls, minimizing public health risks.
Blockchain is being adopted to automate and secure health insurance claims processing. By utilizing smart contracts, claims can be automatically verified and processed, reducing fraud, administrative costs, and processing times. This creates a more transparent and efficient system for payers, providers, and patients. Research indicates that blockchain has the potential to reshape the claims authorization process due to its decentralized and tamper-proof features, along with its consensus protocols.48 During the COVID-19 pandemic, blockchain was employed in various countries to verify vaccination status and medical supply authenticity.49 Other platforms like BurstIQ and Guardtime have developed enterprise-grade tools for secure health data exchange that comply with HIPAA. IBM’s Rapid Supplier Connect, launched in 2020, used blockchain to identify reliable medical suppliers during the early pandemic surge. These real-world examples affirm blockchain’s flexibility and adaptability in diverse healthcare contexts, from clinical trials and claim processing to IoT-based patient monitoring.
Policy Recommendations
To realize the full potential of blockchain in health care, coherent and forward-thinking policy interventions are essential. First, a regulatory “sandbox” should be established to allow for safe experimentation with blockchain technologies. These frameworks, used successfully in the UK and Singapore, enable testing under regulatory oversight without immediate compliance penalties.50
Second, international and national standards must be developed for blockchain data interoperability. Just as HL7-FHIR enabled consistent data sharing across EHRs, a blockchain-FHIR hybrid standard can facilitate distributed healthcare networks. Collaboration between public agencies, standards organizations (e.g., the International Organization for Standardization), and blockchain alliances is needed.
Third, governments should fund pilot programs and infrastructure upgrades. Tax credits, innovation grants, and public-private partnerships can lower the entry barrier for under-resourced providers.
Fourth, blockchain literacy must be embedded into health informatics and policy education. Medical, nursing, and IT schools should offer modules on blockchain ethics, architecture, and governance.
Fifth, data governance frameworks should be updated to reflect patient-centric models. Legal recognition of patient-owned data, smart contract enforceability, and digital identity standards are crucial to building trustworthy systems.
Sixth, to further accelerate the responsible and effective integration of blockchain technology into health care, it is crucial to establish dedicated funding and investment mechanisms, including venture capital incentives and public-private partnerships for infrastructure, alongside increased research and development funds.51 Finally, establishing robust cybersecurity frameworks for blockchain-based systems, encompassing threat intelligence sharing, incident response protocols, and regular security audits, will safeguard sensitive health data.
Conclusions
Blockchain technology represents a powerful solution to many persistent challenges in the healthcare sector. Its inherent capabilities to secure, decentralize, and validate data offer a transformative pathway for managing patient records, optimizing supply chains, and advancing clinical research. Despite the acknowledged technical and regulatory obstacles, successful pilot programs and national initiatives globally have demonstrated blockchain’s feasibility and tangible benefits.31 Strategic adoption, however, necessitates a comprehensive approach that considers technology characteristics, organizational readiness, and environmental factors, emphasizing PU, ease of use, and seamless compatibility with existing healthcare infrastructure.36 Adequate training and robust technical support are also paramount to facilitate a smooth and effective adoption process.
Ultimately, the successful integration of blockchain in health care hinges on careful planning, robust stakeholder alignment, and forward-thinking policy. Collaborative efforts among governments, academic institutions, and industry are crucial to test, standardize, and scale blockchain applications effectively. The potential benefits, ranging from improved patient trust and reduced costs to enhanced efficiency and significant fraud reduction, are too substantial to overlook.52
Future research should strategically focus on developing advanced privacy mechanisms like zero-knowledge proofs, ensuring seamless multi-chain interoperability and establishing robust ethical governance models.53 With coordinated support and continued innovation, blockchain is poised to underpin a resilient, transparent, and equitable global digital health infrastructure.
Contributors
The author is responsible for conceptualization, methodology, validation, data analysis, writing, and editing.
Data Availability Statement (DAS), Data Sharing, Reproducibility, and Data Repositories
All data produced in this study are available upon reasonable request to the corresponding author.
Application of AI-Generated Text or Related Technology
The use of AI to assist with grammar correction, spelling, and editorial refinement throughout the preparation of this manuscript.
References
- Cheikhrouhou O, Mershad K, Laurent M, Koubaa A. Blockchain and emerging technologies for next generation secure healthcare: a comprehensive survey of applications, challenges, and future directions. Blockchain Res Appl. 2025:100305. https://doi.org/10.1016/j.bcra.2025.100305
- Kasyapa MS, Vanmathi C. Blockchain integration in healthcare: a comprehensive investigation of use cases, performance issues, and mitigation strategies. Front Digit Health. 2024;6:1359858. https://doi.org/10.3389/fdgth.2024.1359858
- Bazel MA, Mohammed F, Ahmad M, Baarimah AO, Al Maskari T. Blockchain technology adoption in healthcare: an integrated model. Sci Rep. 2025;15(1):14111. https://doi.org/10.1038/s41598-025-95253-x
- Alsadhan A, Alhogail A, Alsalamah H. Blockchain-based privacy preservation for the internet of medical things: a literature review. Electronics. 2024;13(19):3832. https://doi.org/10.3390/electronics13193832
- AbdelSalam FM. Blockchain revolutionizing healthcare industry: a systematic review of blockchain technology benefits and threats. Perspect Health Inf Manag. 2023;20(3):1b.
- Nakamoto S. Bitcoin: a peer-to-peer electronic cash system. SSRN Electronic Journal. 2008:3440802. https://doi.org/10.2139/ssrn.3440802
- Epiphaniou G, Daly H, Al-Khateeb H. Blockchain and healthcare. In: Blockchain and clinical trial: securing patient data. Cham: Springer International Publishing; 2019, p. 1–29.
- Hughes F, Morrow MJ. Blockchain and health care. Policy Polit Nurs Pract. 2019;20(1):4–7. https://doi.org/10.1177/1527154419833570
- Schiavone F, Omrani N. Innovating responsibly: exploring digital transformation and open innovation strategies. J Innov Econ Manag. 2025;47(2):1–14.
- Wang YM, Wang YS, Yang YF. Understanding the determinants of RFID adoption in the manufacturing industry. Technol Forecast Soc Change. 2010;77(5):803–15.
- Dash S, Gantayat PK, Das RK. Blockchain technology in healthcare: opportunities and challenges. In: Blockchain technology: applications and challenges. 2021, pp. 97–111.
- Mazlan AA, Daud SM, Sam SM, Abas H, Rasid SZ, Yusof MF. Scalability challenges in healthcare blockchain system—a systematic review. IEEE Access. 2020;8:23663–73. https://doi.org/10.1109/ACCESS.2020.2969230
- Agbo CC, Mahmoud QH, Eklund JM. Blockchain technology in healthcare: a systematic review. Healthcare (Basel). 2019;7(2):56. https://doi.org/10.3390/healthcare7020056
- Saeed H, Malik H, Bashir U, Ahmad A, Riaz S, Ilyas M, et al. Blockchain technology in healthcare: a systematic review. PLoS One. 2022;17(4):e0266462. https://doi.org/10.1371/journal.pone.0266462
- Yaqoob I, Salah K, Jayaraman R, Al-Hammadi Y. Blockchain for healthcare data management: opportunities, challenges, and future recommendations. Neural Comput Appl. 2022;34(14):11475–90. https://doi.org/10.1007/s00521-020-05519-w
- Azaria A, Ekblaw A, Vieira T, Lippman A. MedRec: using blockchain for medical data access and permission management. In: 2016 2nd International Conference on Open and Big Data (OBD); 2016 Aug 22–24; Vienna, Austria. IEEE; 2016, pp. 25–30.
- Azogu I, Norta A, Papper I, Longo J, Draheim D. A framework for the adoption of blockchain technology in healthcare information management systems: a case study of Nigeria. In: Proceedings of the 12th International Conference on Theory and Practice of Electronic Governance; 2019 Apr 3–5; Melbourne, Australia. ACM; 2019, pp. 310–6.
- Haleem A, Javaid M, Singh RP, Suman R, Rab S. Blockchain technology applications in healthcare: an overview. Int J Intell Netw. 2021;2:130–9. https://doi.org/10.1016/j.ijin.2021.09.005
- Kuo TT, Kim HE, Ohno-Machado L. Blockchain distributed ledger technologies for biomedical and health care applications. J Am Med Inform Assoc. 2017;24(6):1211–20. https://doi.org/10.1093/jamia/ocx068
- Johar S, Ahmad N, Asher W, Cruickshank H, Durrani A. Research and applied perspective to blockchain technology: a comprehensive survey. Appl Sci. 2021;11(14):6252. https://doi.org/10.3390/app11146252
- Dehghani M, Kennedy RW, Mashatan A, Rese A, Karavidas D. High interest, low adoption: a mixed-method investigation into the factors influencing organisational adoption of blockchain technology. J Bus Res. 2022;149:393–411. https://doi.org/10.1016/j.jbusres.2022.05.015
- Mutambik I, Lee J, Almuqrin A, Alharbi ZH. Identifying the barriers to acceptance of blockchain-based patient-centric data management systems in healthcare. Healthcare (Basel). 2024;12(3):345. https://doi.org/10.3390/healthcare12030345
- Davis FD. Perceived usefulness, perceived ease of use, and user acceptance of information technology. MIS Q. 1989;13(3):319–40. https://doi.org/10.2307/249008
- Marangunić N, Granić A. Technology acceptance model: a literature review from 1986 to 2013. Univers Access Inf Soc. 2015;14(1):81–95. https://doi.org/10.1007/s10209-014-0348-1
- Chatterjee S, Rana NP, Dwivedi YK, Baabdullah AM. Understanding AI adoption in manufacturing and production firms using an integrated TAM-TOE model. Technol Forecast Soc Change. 2021;170:120880. https://doi.org/10.1016/j.techfore.2021.120880
- Tornatzky LG, Fleischer M. The processes of technological innovation. Lexington, MA: Lexington Books; 1990.
- Bach MP, Meško M, Stjepić AM, Khawaja S, Quershi FH. Understanding determinants of management simulation games adoption in higher educational institutions using an integrated technology acceptance model/technology–organisation–environment model: educator perspective. Information. 2025;16(1):45. https://doi.org/10.3390/info16010045
- Bryan JD, Zuva T. A review on TAM and TOE framework progression and how these models integrate. Adv Sci Technol Eng Syst J. 2021;6(3):137–45. https://doi.org/10.25046/aj060316
- Abbate S, Centobelli P, Cerchione R, Oropallo E, Riccio E. Blockchain design in health data management. In: 2022 IEEE Technology and Engineering Management Conference (TEMSCON EUROPE); 2022 Apr 25–27; Nancy, France. IEEE; 2022, pp. 247–53.
- Dehghani M, Popova A, Gheitanchi S. Factors impacting digital transformations of the food industry by adoption of blockchain technology. J Bus Ind Mark. 2022;37(9):1818–34. https://doi.org/10.1108/JBIM-12-2020-0540
- Clohessy T, Acton T. Investigating the influence of organizational factors on blockchain adoption: an innovation theory perspective. Ind Manag Data Syst. 2019;119(7):1457–91. https://doi.org/10.1108/IMDS-08-2018-0365
- Ala’a A, Ramayah T. Predicting the behavioural intention of Jordanian healthcare professionals to use blockchain-based EHR systems: an empirical study. J Syst Manag Sci. 2023;13(4):107–39.
- Mettler M. Blockchain technology in healthcare: the revolution starts here. In: 2016 IEEE 18th International Conference on e-Health Networking, Applications and Services (Healthcom); 2016 Sep 14–16; Munich, Germany. IEEE; 2016, pp. 1–3.
- Ramdani B, Kawalek P, Lorenzo O. Predicting SMEs’ adoption of enterprise systems. J Enterp Inf Manag. 2009;22(1/2):10–24. https://doi.org/10.1108/17410390910922796
- Zhang P, Schmidt DC, White J, Lenz G. Blockchain technology use cases in healthcare. In: Advances in computers. Vol. 111. Amsterdam: Elsevier; 2018, pp. 1–41.
- Malik S, Chadhar M, Vatanasakdakul S, Chetty M. Factors affecting the organizational adoption of blockchain technology: extending the technology–organization–environment (TOE) framework in the Australian context. Sustainability. 2021;13(16):9404. https://doi.org/10.3390/su13169404
- Lee TF, Chang IP, Kung TS. Blockchain-based healthcare information preservation using extended chaotic maps for HIPAA privacy/security regulations. Appl Sci. 2021;11(22):10576. https://doi.org/10.3390/app112210576
- Lee K, Lim K, Jung SY, Ji H, Hong K, Hwang H, et al. Perspectives of patients, health care professionals, and developers toward blockchain-based health information exchange: qualitative study. J Med Internet Res. 2020;22(11):e18582. https://doi.org/10.2196/18582
- Alazab M, Alhyari S, Awajan A, Abdallah AB. Blockchain technology in supply chain management: an empirical study of the factors affecting user adoption/acceptance. Cluster Comput. 2021;24(1):83–101. https://doi.org/10.1007/s10586-020-03200-4
- Gaynor M, Tuttle-Newhall J, Parker J, Patel A, Tang C. Adoption of blockchain in health care. J Med Internet Res. 2020;22(9):e17423. https://doi.org/10.2196/17423
- Malik S, Chadhar M, Chetty M, Vatanasakdakul S. Adoption of blockchain technology: exploring the factors affecting organizational decision. Hum Behav Emerg Technol. 2022;2022:7320526. https://doi.org/10.1155/2022/7320526
- Kimani D, Adams K, Attah-Boakye R, Ullah S, Frecknall-Hughes J, Kim J. Blockchain, business and the fourth industrial revolution: whence, whither, wherefore and how? Technol Forecast Soc Change. 2020;161:120254. https://doi.org/10.1016/j.techfore.2020.120254
- Ben Fekih R, Lahami M. Application of blockchain technology in healthcare: a comprehensive study. In: International Conference on Smart Homes and Health Telematics; 2020 Jun 24–26; Hammamet, Tunisia. Springer; 2020, pp. 268–76.
- Toufaily E, Zalan T, Dhaou SB. A framework of blockchain technology adoption: an investigation of challenges and expected value. Inf Manag. 2021;58(3):103444. https://doi.org/10.1016/j.im.2021.103444
- Lu L, Liang C, Gu D, Ma Y, Xie Y, Zhao S. What advantages of blockchain affect its adoption in the elderly care industry? A study based on the technology–organisation–environment framework. Technol Soc. 2021;67:101786. https://doi.org/10.1016/j.techsoc.2021.101786
- International Comparative Legal Guides. Digital Health Laws and Regulations Report 2024–2025 China [Internet]. London: ICLG; 2024 [cited 2024 Dec 15]. Available from: https://iclg.com/practice-areas/digital-health-laws-and-regulations/china
- Ziegler Y, Uli V, Wortmann J. Blockchain innovation in pharmaceutical use cases: PharmaLedger and Mytigate. J Supply Chain Manag Logist Procure. 2021;3(4):312–25. https://doi.org/10.69554/IPJD9150
- El-Samad W, Atieh M, Adda M. Transforming health insurance claims adjudication with blockchain-based solutions. Procedia Comput Sci. 2023;224:147–54. https://doi.org/10.1016/j.procs.2023.09.022
- Khurshid A. Applying blockchain technology to address the crisis of trust during the COVID-19 pandemic. JMIR Med Inform. 2020;8(9):e20477. https://doi.org/10.2196/20477
- Cheah S, Pattalachinti S, Ho YP. Blockchain industries, regulations and policies in Singapore. Asian Res Policy. 2018;9(2):83–98.
- Al-Khasawneh MA, Faheem M, Alarood AA, Habibullah S, Alzahrani A. A secure blockchain framework for healthcare records management systems. Healthc Technol Lett. 2024;11(6):461–70. https://doi.org/10.1049/htl2.12092
- AbdelSalam FM, Subramaniam C, Silver RA, Turovlin A. Transformative power of IoT, AI, and blockchain in healthcare: an overview. In: The Palgrave handbook of breakthrough technologies in contemporary organisations. Cham: Palgrave Macmillan; 2025, pp. 261–72.
- Chi PW, Lu YH, Guan A. A privacy-preserving zero-knowledge proof for blockchain. IEEE Access. 2023;11:85108–17. https://doi.org/10.1109/ACCESS.2023.3302691
Copyright Ownership: This is an open-access article distributed in accordance with the Creative Commons Attribution Non-Commercial (CC BY-NC 4.0) license, which permits others to distribute, adapt, enhance this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See http://creativecommons.org/licenses/by-nc/4.0. The authors of this article own the copyright.