NARRATIVE/SYSTEMATIC REVIEWS/META-ANALYSIS
Systematic Review of Usability Factors, Models, and Frameworks with Blockchain Integration for Secure Mobile Health (mHealth) Applications
Irum Feroz, PhD1 and Nadeem Ahmad, PhD2
1Department of School of Arts and Creative Technologies, University of Bolton, Bolton, United Kingdom,
2Department of Computing and Technology, Iqra University, H-9 Campus, Islamabad, Pakistan
Keywords: blockchain, mobile health applications, systematic literature review, usability frameworks, usability standards and models
Abstract
This systematic review examines critical usability factors that influence the adoption of mobile health (applications among older adults) and identifies gaps in current usability models, including ISO 9241-11, Nielsen’s heuristics, and Panicoideae, Aristidoideae, Chloridoideae, Micrairoideae, Arundinoideae, Danthonioideae. This review also explores the potential role of blockchain technology in enhancing multimodal medical data systems within mHealth applications. A comprehensive search across six databases yielded 1,073 studies, with 60 meeting the inclusion criteria. Studies were analyzed through thematic synthesis to identify key success factors (RQ1) and comparative analysis to assess limitations in existing frameworks (RQ2). Key factors promoting mHealth adoption included ease of use, efficiency, error prevention, learnability, memorability, and user satisfaction. Blockchain integration emerged as a promising approach to improve data security, interoperability, and user trust, particularly for older adults who engage with complex, multimodal health data. Findings from RQ2 highlighted gaps in usability models, such as the lack of age-specific guidance for multimodal interaction, error recovery, and data privacy. These results underscore the need to define a new usability framework and incorporate blockchain to meet the unique needs of older adults in mHealth applications, supporting both secure and accessible healthcare management.
Plain Language Summary
This review investigates mobile health application’s integration with blockchain. This review explores user-friendly mHealth applications for older adults and also explores how blockchain can improve data systems in these applications. After analyzing 60 studies, key factors for the adoption of information technology were identified, including ease of use, efficiency, error prevention, and user satisfaction. The researchers discovered that blockchain enhances data security, interoperability, and trust of mHealth applications. Moreover, existing usability models lack elderly specific guidance, particularly for handling errors and privacy in mHealth applications. These findings highlight the need for a new usability framework tailored to older adults, integrating blockchain to ensure secure, accessible, and user-friendly healthcare management.
Citation: Blockchain in Healthcare Today 2024, 7: 357.
DOI: https://doi.org/10.30953/bhty.v7.357
Copyright: © 2024 This is an open access article distributed in accordance with the Creative Commons Attribution Non Commercial (CC BY-NC 4.0) license, which permits others to distribute, adapt, enhance this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: http://creativecommons.org/licenses/by-nc/4.0.
Submitted: October 31, 2024; Accepted: November 26, 2024; Published: December 16, 2024
Corresponding Author: Nadeem Ahmad, Email: nadeem.ahmad@ieee.org
Competing interests and funding: There is no conflict of interest between authors.
There is no funding involved in this study.
More than 100,000 mobile health (mHealth) applications are available in the Android and iOS app stores, and this number is continually rising with the rapid development of new applications.1 The mHealth applications demonstrated substantial utility by aiding in prevention, early detection, screening, and public education. These applications became an essential tool in managing the COVID-19 outbreak by offering accessible information and supporting treatment protocols.2 For instance, a symptom tracker app was launched in the United Kingdom to collect self-reported COVID-19 symptoms, enabling the identification of positive cases even among individuals who had not been tested.3
The adoption of information technology in healthcare has effectively addressed gaps in access and quality within healthcare systems.4 Current digital health trends, including mHealth, focus on empowering patients, consumers, clinicians, and researchers with mobile technology to improve overall health outcomes.5,6 Widely used by hospitals, medical students, and allied health workers, mHealth applications facilitate rapid dissemination of health information, news, and critical updates.7–9 These applications enhance medical care and bolster public health by promoting healthy lifestyles and supporting chronic disease management through tools for tracking fitness, diet, diabetes management, and medication adherence. The mHealth market was valued at approximately USD 40 billion in 2020, with an estimated annual growth rate of 17.7% from 2021 to 2028, driven by its ability to improve patient lifestyles and healthcare outcomes.10
According to recent classifications, mHealth applications are categorized into fields such as tracking, communication, decision support, education, awareness, and monitoring.11 These categories reflect the ways mHealth applications cater to the needs of users and healthcare providers, by assisting physicians in selecting applications tailored to specific health conditions (as shown in Table 1).12 Compared to traditional healthcare processes, mHealth applications enhance data collection,13 improve care delivery, foster patient engagement, and allow for real-time monitoring of medications and health metrics.14
| Reference | Sources for defining categories of mHealth applications | Categories |
| Ventola CL. (2014)18 | Use of mHealth devices and apps by healthcare professionals |
|
| Burke, L. et al. (2015)19 | mHealth applications for IOS device developer perspectives |
|
| Industry, N (2015)20 | IMS Institute for Healthcare Informatics (2015), mHealth applications are categorized |
|
| Barton AJ (2012)21 | The Royal Tropical Institute characterized eight mHealth application regions |
|
Despite the growth and potential of mHealth applications, nearly a quarter of these apps remain unused after installation.15 Many applications are developed with insufficient attention to quality or user-centered design (UCD), leading to poor usability, particularly among older adults.16 Blockchain technology, integrated within mHealth applications, offers a solution to some of these challenges.
Blockchain’s decentralized and secure framework can enhance data security, ensure patient privacy, and improve interoperability within multimodal medical data systems. By enabling users to control their data and facilitating seamless data exchange across healthcare platforms, blockchain can increase trust, transparency, and overall user engagement with mHealth applications.17
The integration of blockchain in multimodal data systems can thus address essential usability concerns, particularly for older adults managing complex health conditions through multiple digital platforms. This innovative approach underscores the potential of mHealth to provide efficient, secure healthcare solutions and redefine digital health for a broader, more engaged audience.
Objectives
The primary goal of this literature review is to present studies on mHealth applications, usability guidelines, and European Union (EU) standards for adopting health information technologies, with a specific focus on blockchain integration in multimodal medical data systems. This research addresses the following research questions:
RQ1: Success Factors
What are the critical success factors that enhance the adoption of mHealth applications among older adults, considering their unique needs, preferences, and limitations, and how might blockchain technology support these factors?
RQ2: Gaps in Existing Usability
What are the gaps in existing usability models and guidelines for mHealth applications, particularly concerning the adoption, usability, and security of these applications among older adults in multimodal data environments?
Presented here is a comprehensive systematic literature review (SLR) on usability frameworks and guidelines for mHealth applications, with an emphasis on adoption among older adults and the role of blockchain technology in enhancing usability, security, and data interoperability.
This is followed by a discussion of the eligibility criteria, including inclusion and exclusion parameters, information sources, selection processes, data items, and synthesis methods used in the review. It provides an indepth discussion on RQ1, exploring topics such as acceptance and adherence to digital interventions in mHealth Apps, European Usability Guidelines for Health Information Technologies, and key usability standards and frameworks for developing mobile applications.
Additionally, it discusses the synthesis for RQ2, addressing critical issues including age-related usability challenges, cultural diversity in blockchain integration, the need for empirical evidence in UCD alongside blockchain’s potential, and the gap in comprehensive usability frameworks.
The results section presents details on study selection, characteristics, individual study results, and synthesis findings for both RQ1 and RQ2, following Preferred Reporting Items for Systematic reviews and Meta-Analyses (PRISMA) guidelines.
A discussion of the findings, with suggestions for future research directions to enhance mHealth usability and security for older adults.
Overall, this review provides valuable insights into the usability landscape of mHealth applications, underscoring the need for adaptable frameworks that accommodate the specific needs and data security expectations of older adult users.
Methods
This article presents a SLR of mHealth applications, usability frameworks, and usability guidelines, with a particular focus on integrating blockchain technology for enhanced security and data interoperability in multimodal medical data systems. A total of 60 relevant studies were analyzed to explore usability evaluation frameworks, guidelines, models, and design factors. The review identified that two core approaches significantly influence the success of any software application: usability and user experience (UX). Usability focuses on software efficiency, effectiveness, and user satisfaction, while UX assesses user perceptions and emotional responses through various feedback methods, including questionnaires.
Eligibility Criteria (Section 2)
This systematic review included studies examining mHealth usability and data security, integrating blockchain’s role where applicable. Studies from peer-reviewed journals, conferences, and authoritative usability standards (e.g., International Standardization Organization through the Vienna Agreement (ISO) standards, EU guidelines) were considered. Studies conducted in simulated environments were excluded, as they do not fully represent real-world application scenarios. The eligibility criteria for this review are listed in Table 2.
Information Sources
For the literature review, a thorough search was conducted across multiple online repositories and research databases. The goal was to identify papers that made significant contributions to the usability of healthcare applications. The following library databases were searched:
- Springer Link (https://link.springer.com/)
- Wiley InterScience (www.interscience.wiley.com/)
- Elsevier Science Direct (https://www.sciencedirect.com/)
- Google Scholar (https://scholar.google.com/)
- ACM Digital Library (www.portal.acm.org/dl.cfm)
- IEEE Xplore (https://ieeexplore.ieee.org/Xplore/home.jsp)
The search terms of the strategy were combined with Boolean operators (AND, OR). Search strategy and keyword hits in the databases are given in Table 3. These databases were chosen for their comprehensive coverage of healthcare technology and usability research. Each source was thoroughly explored to ensure that relevant studies on mHealth applications, usability frameworks, and related design factors were identified.
Search Strategy
A well-structured search strategy was employed to retrieve relevant studies. The search terms were carefully selected and combined using Boolean operators (AND, OR) to maximize the relevance of the search results. The keywords and search terms used in this study are summarized in Table 4.
The search strategy was applied across all the databases listed in the Information Sources above, with search queries tailored to the search engine of each database to ensure optimal results. No filters were applied for gender, specific health conditions, or types of applications. This ensured a broad representation of mHealth usability evaluations.
After applying the search strategy, a total of 1,073 papers were identified as potentially relevant. The titles and abstracts of these papers were reviewed to assess their relevance to the research topic. Duplicates were identified and removed using EndNote reference management software, which resulted in the exclusion of 396 duplicate articles. This left 677 papers for the next stage of screening.
Selection Process
The selection process for this systematic review followed a structured and methodical approach. Initially, 1,073 studies were identified through the comprehensive search strategy described earlier. The references were imported into EndNote, where duplicates were automatically removed. This process reduced the number of articles to 677 unique studies.
The selection process was conducted in multiple stages:
Stage 1: Title Screening
The titles of all 677 papers were reviewed by two independent reviewers to assess their relevance to the research topic. This first stage aimed to exclude papers that clearly did not relate to mHealth usability, older adult populations, or usability frameworks/models. After this stage, 607 papers were retained for further review, while 70 papers were excluded for being irrelevant or misleading in their titles.
Stage 2: Abstract Screening
The abstracts of the remaining 607 papers were examined. This stage aimed to eliminate papers that did not explicitly discuss existing or novel frameworks for evaluating the usability of mHealth applications. During this stage, 421 papers were excluded because they focused on individual application designs without significant discussion on usability frameworks, models, or guidelines. Consequently, 186 papers were passed on for full-text review.
Stage 3: Full-Text Review
Full-text versions of the remaining 186 papers were assessed based on the predefined inclusion and exclusion criteria. This stage involved a thorough examination of the methodologies, usability parameters discussed, and relevance to the study objectives. Of these, 126 papers were excluded, as they did not evaluate usability frameworks or models or failed to address the key usability parameters outlined for mHealth applications. A final set of 60 papers was included in the systematic review.
The entire selection process is illustrated in the PRISMA for flow diagram (Figure 1), which shows the steps of identification, screening, eligibility assessment, and final inclusion. This detailed process ensured that only the most relevant studies were included for synthesis.
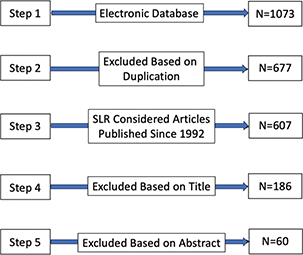
Fig. 1. The selection process of primary papers.
Data Items
The main outcomes of interest in this review were usability metrics critical for evaluating the user-friendliness, security, and effectiveness of mHealth applications, particularly in the context of blockchain-integrated multimodal medical data systems. The primary data items included error prevention, assessing how well applications are designed to minimize user errors, provide clear error messages, and support users in recovering from mistakes. This is especially important in blockchain-enabled systems, where data entries are immutable, and correcting errors may require additional steps.
Another essential metric was learnability, which measured how easily new users could navigate and operate the application, with a focus on blockchain-related features like data privacy settings and transaction transparency. Studies assessing learnability examined the onboarding experience for users in blockchain-integrated environments, as well as the time required to understand these systems’ unique functionalities.
Additional primary data items included memorability, reflecting users’ ability to recall how to use the application after a period of non-use. This metric is particularly relevant for older adults who might interact with mHealth applications intermittently, especially if they need to manage blockchain-based permissions or access controls. User satisfaction was another key outcome, typically gathered through surveys, questionnaires, or qualitative feedback, capturing the overall experience with the application and specific blockchain features that influenced positive or negative perceptions, such as data control and security transparency. Finally, efficiency was measured by the time and effort required to complete tasks within the application, including navigating blockchain-based data verification processes. Efficient design is critical in mHealth applications, as it directly impacts user engagement and sustained usage.
In addition to the primary usability metrics, secondary data items were collected to provide a comprehensive context for mHealth usability, especially within blockchain-integrated systems. These items included participant characteristics, such as age, gender, cognitive abilities, and physical capabilities, with particular attention to older adults who might have unique usability needs in managing blockchain-secured health data.
The specific mHealth application type evaluated in each study was documented, covering areas such as fitness tracking, chronic disease management, mental health support, and medication adherence, especially where these applications incorporated blockchain technology for secure data handling. This categorization helped identify usability challenges unique to each type of health application, particularly in handling sensitive multimodal health data across interconnected platforms.
Another secondary data item was the study context or setting, indicating whether evaluations were conducted in clinical settings, real-world environments, or through remote testing. This context provided insights into how different settings impact usability, especially when blockchain functionality (e.g., secure data sharing) is a key feature.
Additional usability-related factors, including system reliability, ease of navigation, and data security, were recorded. Blockchain was evaluated as a mechanism to enhance data security and user trust, especially concerning privacy control and tamper-resistant data storage. Trust in the application was a crucial factor, as blockchain’s decentralized structure offers transparency, fostering user confidence, especially in sensitive health applications. Finally, the review documented specific usability frameworks and models referenced in each study, such as the ISO 9241-11, Nielsen’s heuristics, and Panicoideae, Aristidoideae, Chloridoideae, Micrairoideae, Arundinoideae, Danthonioideae (PACMAD), comparing their adaptability to blockchain-integrated mHealth applications for older adults.
By systematically collecting and categorizing these primary and secondary data items, this review provides a comprehensive view of the usability landscape for blockchain-enabled mHealth applications. This approach highlights potential improvements in usability frameworks and guidelines tailored to meet the data security and accessibility needs of older adult users in blockchain-integrated medical data systems.
Synthesis Methods
The synthesis for this systematic review was designed to address two research questions: RQ1, identifying critical success factors in the adoption of mHealth applications, and RQ2, analyzing gaps in existing usability models and guidelines for mHealth applications, with a focus on blockchain integration in multimodal medical data systems. Each question was addressed through a structured synthesis process involving thematic categorization and comparative analysis. This approach aimed to distill findings from 60 selected studies, ensuring a comprehensive examination of usability parameters, data security needs, and their implications for mHealth application design, particularly for older adults engaging with blockchain-enabled, multimodal health data systems.
The Synthesis for RQ1
The RQ1 deals with critical success factors in the adoption of mHealth applications (RQ1) and blockchain integration. To address RQ1, studies were selected based on specific criteria to ensure relevance in understanding critical usability success factors for mHealth applications among older adults, especially in contexts that could benefit from blockchain integration in multimodal medical data systems. Only studies that directly assessed usability parameters such as ease of use, efficiency, error prevention, learnability, memorability, and user satisfaction were included. Studies providing quantitative or qualitative assessments of these factors were prioritized, offering a comprehensive view of usability issues older adults face in adopting mHealth applications, particularly those requiring secure and interoperable data management.
For RQ1, a thematic synthesis approach was used to identify and analyze recurring usability themes related to mHealth adoption among older adults, while also considering the potential impact of blockchain-enhanced data security and transparency. Data preparation involved categorizing usability parameters from each study, including ease of use, efficiency, error prevention, learnability, memorability, and user satisfaction. Organizing studies around these parameters enabled a focused analysis on how specific design features and blockchain-integrated data management contribute to user engagement and satisfaction, fostering trust in mHealth applications for older adults. This thematic synthesis revealed how blockchain can support secure, transparent interactions with multimodal health data, thus addressing common usability challenges and enhancing sustained app adoption among older adult populations.
Mobile health refers to the use of mobile communication to manage health and well-being, a term coined by Robert Istepanian.22 The World Health Organization (WHO) defines mHealth as ‘medical and public health practice supported by mobile devices such as mobile phones, personal digital assistants, patient monitoring devices, and other wireless devices’.23 For example, the Global Observation eHealth program highlights the role of mHealth applications in delivering relevant health information and monitoring health statuses for paramedical and support staff.24 The primary aim of mHealth applications is to simplify users’ lives by supporting lifestyle management, nutrition, daily activities, physical exercise, and medication adherence.25 However, many mHealth applications are developed without sufficient consideration of end-user needs,26–28 as they often overlook user requirements and fail to involve users in the design process.29 According to Wildenbos et al., mHealth applications facilitate various aspects of well-being, such as monitoring daily activities, fitness, and disease management. Nonetheless, usability issues are prevalent in many mHealth applications,30 stemming from the lack of comprehensive usability parameters.31
Most existing frameworks primarily focus on the general population or specific user groups, neglecting the specific requirements of older adults.32 Existing usability models and guidelines often overlook age-related cognitive and physical limitations, such as declining memory and visual acuity.33 For instance, Nielsen’s model, widely used in usability evaluations, does not explicitly consider memorability as a usability parameter, which is particularly relevant for older adults who may have difficulties recalling complex interactions.34 The lack of specific guidelines to accommodate these age-related limitations leads to suboptimal usability and low adoption rates among older users. Another notable gap pertains to the usability models’ focus on efficiency and effectiveness, often disregarding factors like learnability, satisfaction, and cognitive load.35 Older adults may require more time and effort to learn how to use mHealth applications effectively, and their satisfaction with the application’s interface and content is crucial for sustained engagement.36 The absence of comprehensive guidelines that consider these usability dimensions impedes older adults’ successful adoption and continued use of mHealth applications. Additionally, the existing usability models and guidelines may not adequately address the privacy and security concerns of older adults when using mHealth applications.37
Blockchain integration in multimodal medical data systems could help address several of these challenges, particularly in supporting user control and data security within mHealth applications. Many applications overlook the unique needs of older users, who often encounter difficulties with login procedures, navigating interfaces, receiving appropriate guidance, managing complex data updates, and ensuring data privacy and security.38 Blockchain’s decentralized framework offers secure, tamper-resistant data management that can address privacy concerns and streamline data access. By enabling secure, interoperable data sharing across devices, blockchain can support user trust and facilitate ease of use in mHealth applications, which is particularly beneficial for older adults managing complex, multimodal health data.
From the literature review, it is evident that existing usability models and guidelines, such as those by Nielsen,34,39 Shneiderman,40 Preece,41,42 Shackel and Constantine,43 and ISO standards,44 do not encompass all aspects of usability. Key usability parameters such as error prevention, learnability, and memorability are often neglected in mHealth frameworks and models.45 In the context of this research, blockchain integration could enhance usability by securely managing health information technologies and addressing critical success factors such as ease of use, efficiency, user satisfaction, motivation, acceptance, trust, and confidence in use.
RQ1 of this research aims to identify the critical success factors that facilitate the adoption of mHealth applications among older adults. The literature reveals that, while mHealth applications play a significant role in health and well-being management, many usability issues stem from inadequate end-user consideration during the design phase. Furthermore, existing usability models lack comprehensive guidelines for older adults. Therefore, critical success factors for mHealth adoption among older users should prioritize usability parameters such as error prevention, learnability, and memorability. Additionally, the potential of blockchain to improve data security, transparency, and interoperability can reinforce ease of use, efficiency, user satisfaction, motivation, acceptance, trust, and confidence, making mHealth applications more adaptable for older adults.
Acceptance and Adherence to Digital Interventions in mhealth Apps
The usability of mHealth applications significantly influences the acceptance and adherence to digital interventions. Designing user-friendly, intuitive, and accessible mHealth apps is essential for catering to a broad audience. Key usability factors include ease of navigation, concise instructions, efficient task completion, and an appealing interface. Prioritizing these usability aspects enhances the overall UX, encouraging users to engage with digital health interventions.46 Integrating blockchain into these systems can further boost user trust, particularly through data transparency and privacy controls, which are essential for sustained engagement among older adults. Blockchain’s secure data framework can reduce the learning curve associated with mHealth applications, increasing acceptance and sustained adherence to digital interventions.
The acceptance of mHealth apps depends heavily on perceived usability. A well-designed, user-friendly interface can instill user confidence, making adoption and continued use more likely.47 Conversely, poor usability often leads to frustration, confusion, and eventual abandonment of the app.29 Thus, usability testing and iterative design processes are crucial to identifying and addressing usability issues, ensuring that mHealth applications meet diverse user needs. By incorporating user feedback throughout development, developers can create applications that align with user expectations, promote acceptance, and foster adherence to digital interventions. Blockchain-enhanced security features can further address user concerns regarding privacy, which is critical for encouraging long-term use, particularly among older adults.
Adherence to digital interventions is closely linked to the usability of mHealth applications. When an app is easy to navigate, provides clear instructions, and offers a seamless UX, individuals are more likely to engage with the intervention consistently and adhere to prescribed protocols. Intuitive features like reminders, personalized notifications, and progress tracking can further enhance adherence by promoting regular usage and providing users with a sense of accomplishment.38 Blockchain technology can support these adherence factors by ensuring that data remain secure, transparent, and accessible to users, empowering them to manage their health data effectively. By recognizing the role of usability and blockchain in facilitating adherence, developers can optimize mHealth applications to support users in achieving improved health outcomes and sustained engagement with digital health interventions.46
European Usability Guidelines in Health Information Technologies
The EU actively supports personalized healthcare through portable and wearable devices. The EU adopted WHO’s definition of mHealth and expanded it to include lifestyle and wellness applications, which may connect to medical devices or sensors, providing personal guidance, health information, and medication reminders via short message service and telemedicine services.48
To address the growing number of mHealth applications in patient care and clinical use, the European Commission published a Green Paper tackling challenges related to mHealth applications within Europe. In April 2014, the Commission launched a dialogue involving healthcare professionals, patients, organizations, and industry representatives to gather insights on the challenges and barriers of mHealth adoption. The Green Paper outlined critical factors impacting the adoption of health information technologies, including data protection, patient safety, equal access, interoperability, liability, data reliability, international cooperation, and quality standards. Blockchain technology, as part of multimodal medical data systems, can play a pivotal role in addressing several of these factors by enhancing data security, interoperability, and patient trust.
Data Protection and Big Data
According to Article 8 of the Charter of Fundamental Rights of the EU and Article 16(1) of the Treaty on the Functioning of the EU, protecting personal data—including health data—is a fundamental right in Europe. With the rapid advancement of mHealth applications, blockchain offers a secure, decentralized approach to data management, reducing risks of unauthorized access and leakage.48 In the context of big data, blockchain can provide a tamper-resistant system that ensures data privacy and integrity, addressing the EU’s focus on secure health-related data collection. Blockchain’s potential for transparent and secure data handling aligns with the eHealth Action Plan 2012–2020, which emphasizes big data protection in health research and innovation.
Patient Safety
The European Parliament’s eHealth Action Plan 2012–2020 emphasizes the importance of well-being and mHealth applications and calls for a clear legal framework to ensure their safe development. Among the 97,000+ mHealth applications globally, blockchain could improve patient safety by offering an immutable record of all health data exchanges. Such transparency can assure users about the source and reliability of data, which is essential given that current mHealth applications often lack information regarding the development processes and adherence to medical guidelines. Safety guidelines focusing on transparency could be further strengthened with blockchain, ensuring the verifiable integrity of mHealth data.
Equal Access and Interoperability
The EU recognizes that the full potential of mHealth applications has yet to be realized in European healthcare. Blockchain’s decentralized nature enables interoperability across platforms, supporting seamless data exchange among healthcare providers and patients, especially across member states. The eHealth Network, developed under Directive 2011/24/EU, enhances interoperability in mHealth systems to maintain high-quality healthcare services across Europe. Blockchain integration would support this initiative by providing a uniform, secure structure for data exchanges that respects patient rights and promotes equal access to health information across borders.
Liability, Reimbursement Model, and Research
Limited innovation and few reimbursement models are key obstacles preventing mHealth applications from becoming mainstream healthcare solutions. National regulations often restrict reimbursements to in-person medical consultations, impeding mHealth adoption. Blockchain could address liability issues by ensuring traceable data transactions, reducing ambiguity over responsibilities related to device faults, IT expertise, or user error. Blockchain’s transparent structure could provide legal clarity in mHealth application development, supporting professionals, developers, and manufacturers in establishing defined responsibilities and accountability for app-related risks.49
Some mHealth applications are popular among the consumer, such as fitness and well-being apps, but there is a need for research to determine whether these applications provide useful information to the users. Research and innovation should be continued on mHealth applications and should continuously cover broader aspects of patient’s safety. The mHealth application’s funding is prioritized in Horizon 202050 EU’s research funding call.
Access and International Cooperation
For effective data privacy and security in mHealth applications, it is critical that the EU follows international standards and fosters collaboration among stakeholders.51 Blockchain’s secure infrastructure could play a significant role in building a platform for experience-sharing, involving entrepreneurs, and advancing mHealth. Existing EU guidelines on data privacy in mHealth applications can be further strengthened with blockchain, ensuring that developers adhere to privacy codes and data protection requirements, which are essential to build user trust. Blockchain provides additional security through data immutability and user control over data sharing, ensuring compliance with the EU’s privacy code of conduct.
Validity and Reliability of Data
To address data validity and reliability, the EU developed specific guidelines in February 2016, involving around 20 organizations to set standards for mHealth data quality. The ability of blockchain to create an immutable, time-stamped record of all interactions supports data validation, ensuring that health data stored in mHealth applications are reliable and verifiable. This system could enhance the EU’s goal of establishing consistent, high-quality data management practices in health applications, ensuring that health providers and patients rely on accurate data for medical decision-making.
Quality Criteria for mhealth and Wellness Applications
The EU’s 2016 Rolling Plan on information and communication technologies (ICT) standardization includes quality criteria for mHealth applications, covering functionality, usability, and reliability. Blockchain can further these standards by securing each step in the application’s development and user interaction cycle, ensuring privacy and transparency. The British Standards Institution developed PAS 277:2015, which recommends quality criteria such as functionality, usability, privacy, and security across the development life cycle. Blockchain enhances compliance with these criteria by offering data integrity, verifiability, and decentralized control, ensuring that mHealth applications meet high standards of reliability, performance, and safety.
Product Safety
The EU Commission is exploring ways to adjust the product safety framework for digital applications, including a public consultation on the safety of mHealth apps. Blockchain integration can contribute to product safety by securing medical data within mHealth systems, ensuring data authenticity and reducing the risk of software tampering or unauthorized data changes.
Supporting Research Under Horizon 2020
Horizon 2020 prioritizes research funding for mHealth innovations, big data, and digital security in health data, providing a foundation for integrating blockchain into secure health data systems. Blockchain can support the EU’s research goals by providing a robust platform for securely managing vast amounts of health data, thereby enhancing the safety, privacy, and functionality of mHealth applications. Adoption of information technology in healthcare would benefit from incorporating EU policy guidelines and blockchain capabilities in mHealth application design and development, addressing security, usability, and transparency for both patients and healthcare providers.
Identifying Parameters from Usability Guidelines and Models
In this theme, usability standards and parameters (metrics) are examined to understand what should be included in the development of a comprehensive usability framework. The objective of usability standards and parameters is to identify factors that contribute to creating user-friendly applications. Preece emphasized that usability is based on observing, experimenting, and testing with users. This research aims to understand users’ specific requirements and define the quality of a skilled experience, as illustrated in Figure 2.52 The International Standards Organization defines usability as the ‘extent to which a product can be used by specified users to achieve specific goals with effectiveness, efficiency, and satisfaction in a specified context of use’.
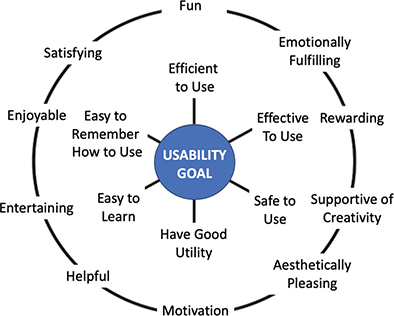
Fig. 2. Usability goals and user experience.52
Over the past 35 years,53 various usability models have been proposed. One of the foundational models was introduced by Shneiderman in his book Designing the User Interface in 1992,40 where he outlined eight golden rules for interface design, including striving for consistency, enabling shortcuts for frequent users, offering informative feedback, designing dialogs to yield closure, providing simple error handling, allowing easy action reversal, supporting an internal locus of control, and reducing short-term memory load. These guidelines were based on the collective experience of developers and aimed at creating intuitive and reliable interfaces.
In 1994, Nielsen34,39 identified five essential usability parameters—efficiency, satisfaction, learnability, memorability, and error handling—arguing that these are vital for software design. Following this, Preece et al.41 introduced classifications that included efficiency, effectiveness, and enjoyment, later expanding to include flexibility, throughput, and learnability.42 These evolving models highlight the importance of creating user-centered applications that are both functional and easy to use.
The ISO further defines usability as the ‘extent to which a product can be used by a specified user to achieve a specified goal with satisfaction, effectiveness, and efficiency in a specified context’.44 Blockchain technology offers an opportunity to enhance these usability models by providing secure, decentralized data handling and improving user control over sensitive health information. For example, blockchain’s immutability and transparency align well with usability goals, fostering user trust and enabling consistent and secure interactions across multimodal health data platforms.
ISO 9241-11 Usability Standard
The ISO 9241-11 standard, established in 1998, provides a framework for measuring usability through decomposed attributes such as effectiveness, efficiency, and satisfaction. Each component is divided into measurable and verifiable sub-components. Blockchain integration could enhance this model by ensuring the data integrity and security of each user interaction, which is especially beneficial in mHealth applications that involve sensitive health data. Blockchain’s decentralized framework ensures that usability is adaptable to different contexts of use, considering factors like users, tasks, equipment, and environments that can affect product usability (Figure 3). By securing data within these contexts, blockchain supports the development of trust-based applications that empower users to manage their data safely and autonomously, aligning with ISO’s principles for context-specific usability.
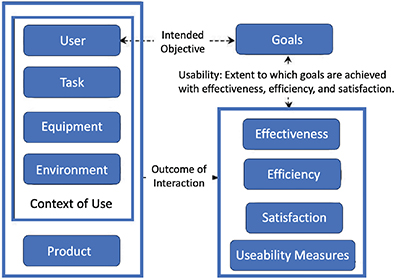
Fig. 3. ISO 9241-11 Usability framework. ISO: International Standardization Organization through the Vienna Agreement.
Georgson and Staggers47 utilized the ISO 9241-11 standard to conduct usability testing among 2,317 patients with diabetes across 18 primary care clinics in the metropolitan area of Utah. The study evaluated task performance, satisfaction, and efficiency, mapping these outcomes to user characteristics. The average satisfaction score of 80.5 indicated good usability, though it left room for improvement. The study also highlighted demographic differences, such as higher task completion rates among males and younger participants. Integrating blockchain technology within such mHealth systems could enhance usability by providing secure, reliable access to health data and supporting patient-centered control over personal health records. Blockchain’s transparent, tamper-resistant data management aligns well with ISO’s emphasis on usability tailored to specific user needs and contexts, as it fosters trust and supports secure interactions within mHealth applications.
ISO 9126-1 Usability Standard
The ISO 9126-1 standard focuses on software product quality, defining both internal/external quality and quality in use. It distinguishes six internal and external quality factors in software usability, which are given in Figure 4. This ISO 9126-1 standard lacks consideration for usability parameters like memorability, learnability, and error handling—areas where blockchain could be instrumental. Blockchain’s secure framework for data verification and integrity complements the ISO 9126-1 standard by enhancing external quality and ensuring data reliability in health applications. This capability is particularly useful for mHealth applications that require dependable data sharing across multiple devices.
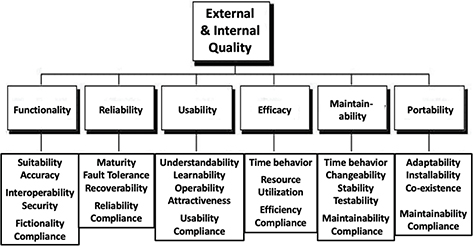
Fig. 4. ISO 9126-1 Usability Framework 2.
Blockchain could also address usability gaps noted in other usability models, such as Nielsen’s, by enhancing data security and error recovery in mHealth applications. For instance, blockchain’s decentralized ledger offers an audit trail for error tracking, which supports error prevention and recovery—critical usability aspects for users managing sensitive health data. Additionally, models like those proposed by Condos et al.54 for mobile commerce applications, which emphasize usability dimensions like content, information architecture, and error prevention, can benefit from blockchain by ensuring secure, consistent data access and reducing the cognitive load on users who interact with these applications in various settings.
The mobile goal question metric (MGQM) model, introduced by Basili et al. in 1994,55 and expanded by Hussain and Kutar,56 is rooted in the ISO 9241-11 standard and assesses usability based on effectiveness, efficiency, and satisfaction. It extends these foundational parameters by introducing six specific usability characteristics: accuracy, attractiveness, features, safety, time taken, and simplicity. The MGQM model leverages both qualitative and quantitative usability metrics, offering a comprehensive framework for evaluating mHealth applications. Integrating blockchain technology within the MGQM framework could enhance data safety and accuracy, two core metrics in MGQM, by ensuring secure, verifiable, and tamper-resistant data transactions. This enhancement could improve user trust and data integrity, especially for older adults managing sensitive health data across multimodal platforms.
PACMAD Usability Model
The PACMAD (People At the Centre of Mobile Application Development) usability model was developed to address limitations in earlier usability models.57 Unlike traditional models, PACMAD integrates both ISO and Nielsen’s usability attributes, adding cognitive load as a critical usability factor for mobile applications. The model identifies three primary components—user, tasks, and context of use—that influence overall usability. Blockchain integration could support PACMAD’s cognitive load considerations by reducing the mental effort needed for data verification and access, as blockchain’s transparent structure simplifies secure data handling. This is especially beneficial for older adults, as it provides secure, controlled access to health information without repeated verifications, lowering cognitive strain.
In mobile applications, the ‘context of use’ is particularly significant, as users may access mHealth applications across different environments and tasks. Blockchain’s decentralized architecture can accommodate these varied contexts by securely sharing data across devices while maintaining user control over data permissions, which aligns with PACMAD’s focus on effectiveness, efficiency, satisfaction, learnability, memorability, error management, and cognitive load summarized in Figure 5. Blockchain-enabled transparency and security can enhance error management and memorability, allowing users to confidently re-engage with mHealth applications over time. Integrating blockchain within usability models like MGQM and PACMAD thus reinforces the usability of mHealth applications, meeting the specific needs of users who rely on secure, interoperable, and user-friendly interfaces for health management.
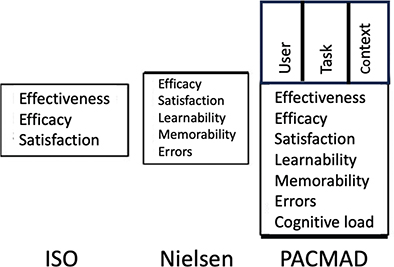
Fig. 5. Comparison of the PACMAD model with other usability models. ISO: International Standardization Organization through the Vienna Agreement; PACMAD: People At the Centre of Mobile Application Development.
The PACMAD model describes the seven attributes as effectiveness, efficiency, satisfaction, learnability, memorability, errors, and cognitive load. All these features have a great impact on usability of application.
Effectiveness: The time a user takes to complete a task in a specific context is called effectiveness. To check if those tasks can be completed in the given time, effectiveness is very necessary.
Efficiency: Efficiency is the ability to complete the project with speed and accuracy. This feature gives a very easy route for the user to use the application. Efficiency can be measured by: Time for the task to be done and keystrokes to get a task done.
Satisfaction: The process of satisfaction is user based, if the given software is comfortable for the user to use and is completely cost effective. This is made for individual users on how well they feel satisfied after using the application. To ask for the reviews of the user, we typically use questionnaires.
Learnability: From a research survey, we have noticed58 that users spend an average of 5 min or less learning to use a mobile application. If an application is not complete and the users using the application face a different problem, they may simply select a different option of application. This attribute was suggested by Nielsen.
Memorability: The research also found that mobile applications are used on a rare basis, and only once a month, 50% of the application used by the participants. Thus, users cannot easily recall how to use the application. Memorability is also suggested by the Nielsen usability model.
Errors: Nielsen defined that users make less error during the use of a system, and if user make errors, they can able to easily improve from them. The usability model PACMAD considers the nature of errors along with the frequency of occurrence, so it is possible to prevent these errors from occurring in future application.
Cognitive load: To use the application, cognitive processing is essential for the user. The common idea of the usability is that the user can perform any task easily without acquiring external help.
In the modern era, users often perform multiple tasks in parallel, which increases cognitive load and poses challenges for usability in mobile applications.58 Developing a self-directed application that effectively serves a technologically unfamiliar target group, such as older adults or individuals with disabilities (e.g., physical disabilities or cognitive impairments like dementia), is especially difficult. Usability becomes critical for these users, as mHealth applications must be intuitive and accessible. Brown et al.45 highlight two key challenges impeding the thorough usability testing of mHealth technology. The first challenge is the limitations of mobile devices, including slow operating systems, low-resolution screens, lack of traditional input devices (like a mouse or keyboard), and inconsistent connectivity. The second challenge is the rapid technological advancements in mHealth, which outpace the development of end-user testing resources and software.
Usability Frameworks for the Development of Mobile Applications
Frameworks contribute toward the administration of usability evaluations by presenting a structured conceptualization of the factors that influence usability and the relations between them. The usability framework of mobile application helps in the development of comprehensive usability evaluation, which involves usability goals, guidelines, metrics, and questions. A framework also contributes toward the evaluation of the usability by presenting structure tools like questionnaires and heuristics. Kaufman et al.59 stated that the frameworks are considered as a set of principles (such as assumptions, constructs, quality criteria, and ideas that guide research and development) and strategies (such as hands-on guidelines, design heuristics, and methods to assist the development process to increase the quality of eHealth technology).60 Some existing frameworks61 such as Health IT Usability Evaluation Model (ITUEM) were introduced by Yen in 201062, and the main purpose was to identify the gap and problems in prior usability models. According to Brown III et al.,45 the Health–ITUEM framework offers to understand the usability issues and barriers related to mHealth technology. The authors used nine concepts in the Health-ITUEM framework, for example, error prevention, completeness, memorability, information needs, flexibility/customizability, learnability, performance speed, and competency for evaluating the usability of the mHealth applications and developing the data analysis codes.63,64
Wildenbos et al. in 2018 developed the MOLD-US framework, which identified four aging barriers, such as cognition, less motivation, perception, and physical abilities.65 Another framework is Information System Research (ISR), which is used as a guideline for the designing mHealth applications.27 The ISR framework is an iterative process, which includes functional requirement identification, need assessment, rapid prototyping, and user interface design, each of these techniques have been used for the development of the software in the past. It consists of three cycles, that is, relevance (in which the focus is on target end-user), rigor (identify the technology), and design (usability-based method involved). The ISR framework also identifies that the user_centered design process is effective in designing m_health applications. It also includes both end-user feedback (focus groups, participatory design sessions, and usability evaluation methods) and multiple UCD methods to update the design of mHealth applications.27,28 The MGQM defines the user goals,55 refines the goals into questions, and defines the metric, which provides information to answer the questions. MGQM is a generic model, which can be used for the measurement of issues in mobile applications.66 Wildenbos et al. in 2018 introduced a framework for the analysis of the usability of mHealth applications for the older people, in which their analysis suggested that learnability and poor visual acuity were the most common issues that affected motivation for the adoption of mHealth applications in older people.67 In this regard, the evaluation of existing usability guideline for mHealth does not address age-related cognitive limitations, motivational issues as a psychological construct, perception (such as small font size on-screen),46 and physical impairment, which is commonly associated with older people65 that resulted in poor adoption of the technology.
Electronic health records (EHRs) are unsystematic due to the lack of usability frameworks.67 Jiajie and Muhammad in 2011 presented a unified framework for EHR usability, which is based on four important usability components, such as task, user, representation, and function (TURF).68 The author stated that usability can not only be defined scientifically under a coherent unified framework but should be measured objectively and systematically. This research defines how TURF can be used to improve the usability of EHRs and also increase their efficiency. In subsequent sections, the gaps that existed in relevant studies are presented.
Synthesis for RQ2
The RQ2 deals with gaps in existing usability models and guidelines. For RQ2, studies were selected based on their evaluation of usability models and guidelines relevant to digital health applications, with a focus on frameworks such as ISO 9241-11, Nielsen’s heuristics, and the PACMAD model. Studies that highlighted specific gaps or limitations in these frameworks when applied to mHealth applications, particularly for older adults, were prioritized. This selection allowed for a comparative analysis to assess how well current models address—or fail to address—the usability needs of older adults.
A structured comparative analysis of these models was conducted to evaluate their strengths and limitations in addressing unique usability requirements for older adults in mHealth applications. Data preparation involved organizing studies by the usability model evaluated and extracting key information on each model’s strengths, limitations, and applicability to mHealth. This organization enabled a direct comparison across frameworks, focusing on usability aspects like error prevention, learnability, multimodal interaction, and cognitive load management. The comparative synthesis identified areas where existing models lack specific guidance for older users, offering insights into how usability frameworks could be adapted or expanded to better meet this demographic’s needs.
Blockchain integration within mHealth applications could address some of these identified gaps by enhancing data security, simplifying user authentication processes, and supporting seamless interoperability, all of which contribute to usability. For instance, ISO 9241-11 emphasizes effectiveness, efficiency, and satisfaction, yet it lacks specific provisions for user-centered data control and transparency—elements that blockchain could improve by allowing users to securely manage and track access to their health data across platforms. Blockchain’s secure, decentralized framework supports trust and control over data, which are crucial for older adults who may have concerns about privacy and security in digital health systems.
Nielsen’s heuristics provide foundational principles for usability, including error prevention and user satisfaction, but they fall short in addressing multimodal interaction and adaptive support tailored to older adults’ needs. Blockchain’s transparent, tamper-resistant data handling could mitigate these issues by ensuring secure data exchanges across devices and enabling consistent, traceable interactions, thus supporting ease of use and reducing the cognitive burden associated with managing health information.
The PACMAD model incorporates cognitive load considerations and aligns with blockchain’s potential for simplifying data handling, particularly in contexts that require multiple devices and secure controlled data interactions. Blockchain’s capability to streamline data management processes could help minimize cognitive load, making mHealth applications more accessible to older adults and improving their overall usability experience.
Overall, the comparative synthesis emphasizes the need to adapt existing usability frameworks to address older adults’ unique usability requirements. Many mHealth applications are designed with insufficient end-user consideration,26–28 and research indicates a lack of user involvement in the design process. Usability, as defined by the ISO standard, involves ‘the effectiveness, efficiency, and satisfaction with which a specified user achieves specified goals in a particular environment’. This is essential to ensure users can perform tasks effectively, as dissatisfaction with an interface can impact market acceptance. Complex interfaces have been shown to reduce user interest and engagement when performing tasks.40 Blockchain integration offers a promising solution by enhancing data security, transparency, and user control, thus potentially addressing many of the usability challenges that persist in existing frameworks.
Age-related Usability Issues
In the current market, the majority of mobile devices use touchscreen technology, a transition from traditional physical buttons that can be confusing for many users, especially older adults. While screen-based buttons and display icons are effective in modern design, they are often not optimized for individuals with disabilities. Although features such as adjustable font sizes can help mitigate vision-related issues, many usability challenges remain, which require a comprehensive approach to address.30 Research has identified specific capabilities and limitations of older adults when interacting with mobile technology, leading to the recommendation of key design principles that can better meet this population’s needs. By incorporating these insights into interface design, developers can create applications that are more accessible and user-friendly for older adults.65
Blockchain technology can further enhance usability for older adults by offering simplified and secure data interactions, which are essential for maintaining user trust in mHealth applications. For instance, blockchain’s transparent, decentralized framework reduces the complexity associated with traditional data management systems, allowing older users to manage health data securely without complex authentication steps. This design approach supports user independence and minimizes the cognitive load, making mHealth applications more suitable for older adults dealing with age-related usability issues.
Cultural Diversity and Blockchain Integration
Culturally diverse environments pose additional challenges in identifying frequently used features and managing applications in multiple languages. Wildenbos et al. emphasize the importance of online navigation structures that cater to diverse cultural behaviors and preferences.65 Kim et al. argue that cultural usability is as essential as any other usability factor when designing effective systems.69 Studies by Ahmad et al.70 highlight the significance of usability problems in many mHealth applications and emphasize the need for comprehensive usability frameworks to address the unique needs of older users. Another important factor is user involvement in the design process. Studies such as Saparamadu et al.71 and Duque et al.72 emphasize that involving older adults in the development and design of mHealth applications leads to better alignment with their requirements and preferences. By engaging older users throughout the development cycle, developers can gain valuable insights into their needs and challenges, resulting in more user-centered applications that are more likely to be adopted.
Designers must consider cultural norms, societal impacts, beliefs, trends, and perceptions to create user-friendly, culturally adaptive applications.27,73 Research reveals that language differences may necessitate significant technical adjustments in software development, highlighting the need for adaptive and context-aware designs.74 Blockchain technology can support these diverse needs by providing a standardized yet secure data management framework that accommodates multi-language interfaces and culturally specific interactions, enhancing cross-cultural usability and reducing the technical complexity associated with localization.
Blockchain’s decentralized nature can also help address back-compatibility issues by offering a consistent, secure data structure that remains accessible across different cultural and linguistic contexts. This universal data format can facilitate market solutions adaptable to diverse user bases, enhancing accessibility and ensuring that mHealth applications are suitable for a variety of cultural backgrounds.
Lack of Empirical Evidence in UCD and Blockchain’s Potential
Khan and Donthula point out that while UCD enhances the commercial success of products, more research is needed to quantify its economic benefits, such as increased sales, customer loyalty, and user engagement.25,75 They recommend further studies to evaluate UCD’s impact on fostering innovation and promoting collaboration between designers, developers, and users. Blockchain’s integration could complement UCD by adding a layer of security and data transparency that aligns with UCD principles, supporting user trust and engagement in mHealth applications. Blockchain enables secure, user-centered data control, allowing end-users more autonomy over their health information while maintaining the privacy and integrity of their data.
Research exploring the combined impact of UCD and blockchain on product success, user satisfaction, and trust could provide valuable insights into optimizing UCD implementation. Blockchain’s transparent and user-controlled data management framework could further support the UCD approach, fostering a collaborative development process that prioritizes end-user needs in digital health solutions.
Lack of Comprehensive Usability Framework
Saleh and Ismail emphasized the need for consistent usability guidelines and standards across various systems and contexts, which includes interaction, visual, and content design standards, as well as ISO 9241 for usability evaluation and improvement.27,75 They suggested that usability frameworks should consider user characteristics—such as age, education level, and cultural background—and should be based on clear usability goals to assess design success and guide improvements. Integrating these elements, they argued, would help designers create systems that are effective, efficient, and satisfying for users.75
Gupta et al.31 highlighted a major challenge in evaluating mHealth applications: the absence of a comprehensive usability framework specifically for mHealth, despite its potential to improve health outcomes. They noted a lack of consensus on effective quality models and usability frameworks for mHealth, which complicates evaluating these applications and ensuring they meet user needs. The authors called for further research to identify the most appropriate usability frameworks to support the user-centered mHealth application design.31 Table 5 highlights research gaps in mHealth applications, including the needs for user-centered and inclusive design, comprehensive usability frameworks, and tailored guidelines for older adults. It also notes limitations in current evaluation models, such as high costs and limited user input.
| Relevant studies | Gaps identified |
| Khan K, and Donthula S (2019)21 | There is still need for further research directed at how user-centered design is contributing to the development of helpful applications. |
| Liew MS et al. (2019)76 | A need to identify gaps regarding mobile application’s inclusive design, assessment from subject experts, and feedback from consumers. |
| Schnall R et al, 201673 | The ISR framework presented by the authors provided some guidelines for designing mHealth applications. The major drawback in the ISR framework is that it can be time-consuming and costly. |
| Wildenbos et al. (2015)30 | The existing mHealth’s guidelines do not address the barriers related to the complexity of mobile interfaces, which cause problems for old age patients. Need to identify gaps regarding mobile application’s inclusive design, assessment from subject experts, and feedback from consumers. |
| Yen PY, and Bakken S. (2012)63 | The researcher and the developers need to use the automatic evaluation tools for identifying the usability barriers as the existing 73% of people’s research is based on the interviews and questionnaires for the evaluation of the mHealth applications, which are more error-prone. |
| Saleh AM, and Ismail RB (2015)75 | The comprehensive usability framework should be based on the usability model, guidelines, characteristics, and goals. |
| Gupta et al. (2014)31 | For the evaluation of mHealth applications, the main challenge is the selection of quality models and inadequate support of appropriate comprehensive usability framework for designing. |
| Tahir R, and Arif F. (2014)43 | From the literature review, the existing usability models or guidelines such as ISO standards do not cover all aspects of usability. |
| Brown et al. (2013),45 | The Health IT Usability Evaluation Model was introduced with the primary purpose of identifying the gaps and problems in prior usability models. The drawback of this framework is that few users were involved in the data collection process, while the framework is not tested. |
| Li C, et al. (2021)77 | There is a lack of specific usability guidelines for mHealth applications targeted at older adults, considering their unique needs and limitations. |
| Hussain A, Kutar M (2012)78 | Existing usability models for mHealth applications often do not adequately address the cognitive limitations and accessibility challenges faced by older adults, hindering their adoption and usability. |
| Slade M, Oades L, and Jarden A (2017)16 | The current usability frameworks for mHealth applications do not fully consider the social and emotional aspects of older adults’ experiences, which can impact their motivation to use these applications. |
| ISR: Information System Research; mHealth: mobile health. | |
Blockchain integration within usability frameworks could address some of these challenges by providing secure, transparent data management and consistent standards across devices. Blockchain’s decentralized approach promotes user trust and control over health data, supporting usability in diverse user contexts and enabling the development of more reliable, user-focused mHealth solutions.
A review of various research papers revealed that no relevant study in the last two decades has introduced a comprehensive usability evaluation framework.46 Such a framework should encompass usability models, guidelines, characteristics, and goals to be effective.75 There is an urgent need to design a usability framework that specifically ensures mHealth applications are developed with older users in mind. Each feature of mHealth applications should be tailored to meet users’ actual needs, expectations, and characteristics, promoting a more user-centered approach in mHealth design.46
Results
Study Selection
The study selection process was conducted according to the structured screening and eligibility criteria outlined in the PRISMA flow diagram (Figure 1). A comprehensive search across multiple databases identified 1,073 records. After removing duplicates, 677 unique records were screened based on their titles and abstracts. From this, 491 records were excluded as they did not meet the initial inclusion criteria, leaving 186 full-text articles for detailed evaluation. A further assessment based on predefined eligibility criteria led to the exclusion of 126 studies, primarily due to reasons such as lack of focus on usability, irrelevant populations (non-older adults), or insufficient emphasis on mHealth applications. Ultimately, 60 studies met all inclusion criteria and were selected for synthesis, addressing the research questions related to usability factors and gaps in existing frameworks.
Study Characteristics
The selected studies, published between 1992 and 2023, demonstrate the evolving focus on mHealth applications, particularly for improving health management, chronic disease monitoring, mental health support, and lifestyle wellness among older adults. Geographically, these studies included significant contributions from North America, Europe, and Asia. Sample sizes varied widely, with smaller focus groups in qualitative studies and larger quantitative studies, some involving thousands of participants in clinical or observational settings.
The study designs included diverse methodologies, such as qualitative evaluations, controlled experiments, usability testing, and cross-sectional surveys. Most studies concentrated on usability parameters like learnability, error prevention, and user satisfaction, while some specifically assessed adherence and retention of older adults using mHealth applications. Additionally, several studies referenced specific usability frameworks, such as ISO 9241-11, Nielsen’s heuristics, and the PACMAD model, to examine usability gaps in current models when applied to mHealth.
The key findings from individual studies are summarized in Table 6, illustrating how each contributes to identifying critical success factors and usability gaps in mHealth applications for older adults. The findings were mapped to specific usability parameters, including ease of use, learnability, error prevention, efficiency, and satisfaction.
| Reference | Findings |
| Feroz I, Ahmad N (2022)5 | Simple, well-labeled icons reduced cognitive load for older adults, resulting in improved task completion rates and greater ease of use. |
| Ahmad N (2014)29 | Navigation and efficient workflows led to higher user satisfaction and more frequent app engagement among users. |
| Ahmad et al. (2015)79 | Consistent layout and familiar visual cues improved memorability, minimizing the need for re-learning after periods of non-use. |
| Harrison R, Flood D, Duce D (2013)57 | Evaluation of the ISO 9241-11 framework in mHealth applications revealed that while it supports general usability metrics, it lacks specific guidance for error recovery. |
| Feroz I (2023)66 | Assessment of Nielsen’s heuristics identified gaps in addressing age-related usability needs, such as visual acuity adjustments and simplified navigation for older adults. |
Results of Individual Studies
Key findings from individual studies are summarized in Table 7, highlighting how each study contributes to understanding the critical success factors and usability gaps in mHealth applications for older adults. Each study’s findings were mapped to specific usability parameters, such as ease of use, learnability, error prevention, efficiency, and satisfaction.
Table 3 provides a summary of study gaps identified in existing literature on mHealth applications. Key gaps include the need for UCD research, inclusive design assessments, and comprehensive usability frameworks that address cognitive, accessibility, and emotional needs—particularly for older adults. Additionally, issues with current evaluation models, such as high costs, limited user involvement, and outdated frameworks, are highlighted.
Results of Syntheses
RQ1: Identifying Critical Success Factors in mHealth Adoption
The thematic synthesis for RQ1 identified several usability factors essential for the adoption and sustained use of mHealth applications among older adults. Key factors included ease of use, efficiency, error prevention, learnability, memorability, user satisfaction, motivation, acceptance, trust, and confidence in app usage. Studies consistently showed that applications with simple navigation, intuitive layouts, and age-friendly visual elements resulted in higher satisfaction and engagement. Efficiency, achieved through streamlined workflows and minimal task steps, emerged as particularly important for older adults who may have limited patience or cognitive capacity for complex interfaces.
Integrating blockchain technology into mHealth applications could further enhance these usability factors by offering secure, user-controlled data management, which builds trust and confidence in app usage. Blockchain’s transparent, decentralized framework supports error prevention by providing tamper-resistant data management, enabling users to verify data accuracy and ensuring data integrity across devices. This security can reduce user frustration and boost confidence, especially for older users concerned with privacy and security. Prioritizing both usability and blockchain’s data security features can create a UCD that encourages sustained engagement and facilitates effective health management for older adults.
Rq2: Analyzing Gaps in Existing Usability Models and Guidelines
The comparative analysis for RQ2 identified several limitations in current usability models, including ISO 9241-11, Nielsen’s heuristics, and PACMAD, when applied to mHealth applications. Existing models often lack age-specific guidance and fail to address critical usability aspects such as multimodal support (e.g., voice commands and haptic feedback), error recovery, and data privacy. Studies indicated that while these frameworks provide foundational usability principles, they do not offer specific recommendations for features that would improve usability for older adults, such as adjustable font sizes, simplified interfaces, and adaptive help tools.
Blockchain integration could address some of these gaps by providing secure, decentralized data management that improves user trust and control over sensitive information. Blockchain’s tamper-resistant data structure supports error recovery by ensuring that all data interactions are transparent and traceable, which is particularly beneficial for older adults concerned about privacy and data security. Additionally, by enabling consistent data access across devices, blockchain could facilitate multimodal interaction options, supporting usability frameworks in expanding their scope to include age-sensitive, accessible mHealth design.
Discussion And Future Work
This SLR highlights that mHealth applications support various aspects of well-being but face usability challenges in parameters such as error prevention, learnability, and memorability. These gaps are particularly problematic for older adults, who may have limited familiarity with information and communication technologies, impacting their adoption and sustained use of mHealth applications.74
Existing usability guidelines for mobile applications76 lack a comprehensive framework specific to mHealth, especially one that considers the needs of older adults. Addressing these gaps requires the development of a new usability framework that incorporates overlooked metrics and adapts to the unique requirements of this demographic.46 Integrating blockchain into this framework could significantly enhance usability by providing secure, user-controlled data management and transparent, tamper-resistant records. Blockchain’s capabilities support error prevention by ensuring data accuracy and traceability, building trust and reducing user anxiety around privacy and security.
Future work should explore usability frameworks that combine these usability principles with blockchain’s security features, allowing older users to interact with mHealth applications confidently. This approach could create more accessible, user-centered mHealth solutions, fostering higher engagement and better health outcomes for older adults.
Contributors
Ms. Irum Feroz contributed significantly in SLR and selected 60 papers after a thorough analysis. She worked on usability factors, models, and frameworks. She found important factors involved in IT adoption. She also identified critical research gaps, highlighted emerging trends and potential areas for further investigation, and provided valuable insights to guide the direction of future research. Mr. Nadeem Ahmad worked on synthesis of research questions and followed PRISMA guidelines. He also worked on integration of mHealth applications with blockchain technology.
All authors approved the manuscript and agree with its submission to Blockchain in Healthcare Today
Data Availability Statement (Das), Data Sharing, Reproducibility, And Data Repositories
The data presented in the study are available with the corresponding author.
Application Of Generated Text Or Related Technology
Artificial intelligence and related technologies were not used in the preparation of this article.
Acknowledgments
We sincerely acknowledge the University of Portsmouth, UK, for providing a supportive and conducive environment that greatly facilitated the successful completion of this research. The resources, infrastructure, and academic encouragement offered by the institution were invaluable in advancing our work.
References
- Pires IM, Marques G, Garcia NM, Flórez-Revuelta F, Ponciano V, Oniani S. A research on the classification and applicability of the mobile health applications. J Pers Med. 2020;10(1):11. https://doi.org/10.3390/jpm10010011
- Asadzadeh A, Kalankesh LR. A scope of mobile health solutions in COVID-19 pandemics. Inform Med Unlocked. 2021;23(100558):100558. https://doi.org/10.1016/j.imu.2021.100558
- Drew DA, Nguyen LH, Steves CJ, Wolf J, Spector TD, Chan AT. Rapid implementation of mobile technology for real-time epidemiology of COVID-19. bioRxiv. 2020. https://doi.org/10.1101/2020.04.02.20051334
- Istepanian RS, Alanzi T. Mobile Health (m-Health): evidence-based progress or scientific retrogression biomedical information technology. Elsevier; 2020.
- Feroz I, Ahmad N. Usability based rating scale (UBRS) for evaluation of mobile health (mHealth) applications. HCI and beyond: advances towards smart and interconnected environments. Vol. 2.
- Marques ICP, Ferreira JJM. Digital transformation in the area of health: systematic review of 45 years of evolution. Health Technol (Berl). 2020;10(3):575–86. https://doi.org/10.1007/s12553-019-00402-8
- Vinay K, Vishal K. Smartphone applications for medical students and professionals. Nitte Univ J Health Sci. 2013;3(1):59–62.
- Jebraeily M, Fazlollahi Z, Rahimi B. The most common smartphone applications used by medical students and barriers of using them. Acta Inform Med. 2017;25(4):232. https://doi.org/10.5455/aim.2017.25.232-235
- Mohapatra D, Mohapatra M, Chittoria R, Friji M, Kumar S. The scope of mobile devices in health care and medical education. Int J Adv Med Health Res. 2015;2(1):3. https://doi.org/10.4103/2349-4220.159113
- MHealth market size, share & trends analysis report by component (wearables, mHealth apps), by services (monitoring services, diagnosis services), by participants, by region, and segment forecasts, 2024–2030. Grandviewresearch.com [cited 2024 Jan 02]. Available from: https://www.grandviewresearch.com/industry-analysis/mhealth-market
- Research2guidance.com. [cited 2024 Jan 02]. Available from: https://research2guidance.com/wp-content/uploads/woocommerce_uploads/2016/10/r2g-mHealth-App-Developer-Economics-2016
- Sezgin E, Özkan-Yildirim S, Yildirim S. Investigation of physicians’ awareness and use of mHealth apps: a mixed method study. Health Policy Technol. 2017;6(3):251–67. https://doi.org/10.1016/j.hlpt.2017.07.007
- Ahmad N, Feroz I, Ahmad F. Creating synthetic test data by Generative Adversarial Networks (GANs) for Mobile Health (mHealth) applications. In International conference on forthcoming networks and sustainability in the AIoT Era 2024 Jan 27 (pp. 322–32). Cham: Springer Nature Switzerland.
- Tomlinson M, Rotheram-Borus MJ, Swartz L, Tsai AC. Scaling up mHealth: where is the evidence? PLoS Med. 2013;10(2):e1001382. https://doi.org/10.1371/journal.pmed.1001382
- Nouri R, R Niakan Kalhori S, Ghazisaeedi M, Marchand G, Yasini M. Criteria for assessing the quality of mHealth apps: a systematic review. J Am Med Inform Assoc. 2018;25(8):1089–98. https://doi.org/10.1093/jamia/ocy050
- Slade M, Oades L, Jarden A. Wellbeing, recovery and mental health. Cambridge University Press; 2017.
- Costa VK, Sias Rodrigues A, Agostini LB, Machado M, Darley N, Cunha Cardosa R. The potential of user experience (UX) as an approach of evaluation in tangible user interfaces (TUI). In: Design, user experience, and usability. Practice and case studies. Springer International Publishing, 2019; p. 30–48.
- Ventola CL. Mobile devices and apps for health care professionals: uses and benefits. P T. 2014;39(5):356–64.
- Burke LE, Ma J, Azar KMJ, Bennett GG, Peterson ED, Zheng Y. Current science on consumer use of mobile health for cardiovascular disease prevention: a scientific statement from the American heart association. Circulation. 2015;132(12):1157–213. https://doi.org/10.1161/CIR.0000000000000232
- Industry News. IMS health study: Patient adoption of mHealth. Health IT answers. Published October 6, 2015 [cited 2024 Jan 04]. Available from: https://www.healthitanswers.net/ims-health-study-patient-adoption-of-mhealth-2/
- Barton AJ. The regulation of mobile health applications. BMC Med. 2012;10(1). https://doi.org/10.1186/1741-7015-10-46
- Istepanian RSH, Pattichis CS, Laxminarayan S. Ubiquitous M-health systems and the convergence towards 4G mobile technologies. In: M-Health. Springer US; 2007:3–14.
- Martínez-Pérez B, de la Torre-Díez I, López-Coronado M. Mobile health applications for the most prevalent conditions by the World Health Organization: review and analysis. J Med Internet Res. 2013;15(6):e120. https://doi.org/10.2196/jmir.2600
- World Health Organization. Global Diffusion of EHealth: making universal health coverage achievable: report of the third global survey on EHealth. World Health Organization.; 2017.
- Khan K, Donthula S. Investigating motivational and usability issues of mHealth wellness apps for improved user experience. In: Advances in intelligent systems and computing. Springer Singapore; 2019:573–87.
- Craven MP, Lang AR, Martin JL. Developing mHealth apps with researchers: multi-stakeholder design considerations. In: Design, user experience, and usability. User experience design for everyday life applications and services. Springer International Publishing, 2014; 15–24.
- Schnall R, Rojas M, Bakken S, Brown W, Carballo-Dieguez A, Carry M. A user-centered model for designing consumer mobile health (mHealth) applications (apps). J Biomed Inform. 2016;60:243–51. https://doi.org/10.1016/j.jbi.2016.02.002
- Feroz I, Ahmad N, Iqbal MW. Usability based rating scale for mobile health applications. In: 2019 International Conference on Engineering and Emerging Technologies (ICEET). IEEE; 2019.
- Ahmad N. People centered HMI’s for deaf and functionally illiterate users. Doctoral dissertation, Universität Potsdam.
- Wildenbos GA, Peute LW, Jaspers MWM. A framework for evaluating mHealth tools for Older Patients on Usability. Stud Health Technol Inform. 2015;210:783–7.
- Gupta D, Ahlawat A, Sagar K. A critical analysis of a hierarchy based Usability Model. In: 2014 International Conference on Contemporary Computing and Informatics (IC3I). IEEE; 2014.
- Amanda G, Layman CV. Examining the intention to use mobile health applications amongst Indonesians. Milestone J Strategic Manag. 2022;2(2):103. https://doi.org/10.19166/ms.v2i2.5924
- Heinz M, Martin P, Margrett JA, Yearns M, Franke W, Yang H-I. Perceptions of technology among older adults. J Gerontol Nurs. 2013;39(1):42–51. https://doi.org/10.3928/00989134-20121204-0
- Nielsen J. Usability engineering. Morgan Kaufmann; 1994 [cited 2024 Nov 30]. Available from: https://www.amazon.com/dp/0125184069?tag=useitcomusablein
- Pfeil U, Zaphiris P, Wilson S. Older adults’ perceptions and experiences of online social support. Interact Comput. 2009;21(3):159–72. https://doi.org/10.1016/j.intcom.2008.12.001
- Selwyn N, Gorard S, Furlong J, Madden L. Older adults’ use of information and communications technology in everyday life. Ageing Soc. 2003;23(5):561–82. https://doi.org/10.1017/s0144686x03001302
- Sixsmith A, Sixsmith J. Ageing in place in the United Kingdom. Ageing Int. 2008;32(3):219–35. https://doi.org/10.1007/s12126-008-9019-y
- Feroz I, Good A, Omisade O. Identification of critical success factors in adoption of health IT services from older people’s perspective. Paper presented at. In: The Proceedings of the 2023 3rd international conference on human machine interaction. 2023.
- Kaplan K. Usability 101: Introduction to usability. Nielsen Norman Group. [cited 2024 Jan 03]. Available from: https://www.nngroup.com/articles/usability-101-introduction-to-usability/.
- Shneiderman B. Designing the user interface: strategies for effective human-computer interaction. Addison-Wesley; 1992.
- Preece J, Benyon D. Open University, a guide to usability: human factors in computing. Addison-Wesley Longman Publishing Co., Inc; 1993.
- Preece J. Citizen science: new research challenges for human–computer interaction. Int J Hum Comput Interact. 2016;32(8):585–612. https://doi.org/10.1080/10447318.2016.1194153
- Tahir R, Arif F. Framework for evaluating the usability of mobile educational applications for children. Society of Digital Information and Wireless Communications. 2014; p. 156–70.
- Alzahrani A, Gay V, Alturki R. The evaluation of usability in mobile applications. In: Proceedings of the 40th International Business Information Management Association (IBIMA). 2022; p. 23–4.
- Brown W 3rd, Yen PY, Rojas M, Schnall R. Assessment of the Health IT Usability Evaluation Model (Health-ITUEM) for evaluating mobile health (mHealth) technology. J Biomed Inform. 2013;46(6):1080–7. https://doi.org/10.1016/j.jbi.2013.08.001
- Feroz I. Developing a usability guidance framework for design and evaluation of mHealth apps for aging populations. Doctoral dissertation, University of Portsmouth. 2023.
- Georgsson M, Staggers N. Quantifying usability: an evaluation of a diabetes mHealth system on effectiveness, efficiency, and satisfaction metrics with associated user characteristics. J Am Med Inform Assoc. 2016;23(1):5–11. https://doi.org/10.1093/jamia/ocv099
- Commission E. Green Paper on Mobile Health (‘m-Health). 2014.
- Informatics I. Patient apps for improved healthcare: from novelty to mainstream. In: Report by the IMS Institute for Healthcare Informatics. 2013.
- Streitenberger W. The new EU regional policy: fostering research and innovation in Europe. Territorial Cohesion in Europe. Pécs: Hungarian Academy of Sciences,2013; p. 36–45.
- Kay M, Santos J, Takane M. mHealth: New horizons for health through mobile technologies. World Health Organization. 2011;64(7):66–71.
- Preece J, Rogers Y, Sharp H. Interaction design: beyond human-computer interaction. John Wiley & Sons; 2002.
- Adibi S, ed. Mobile health: a technology road map. 2015th ed. Springer International Publishing; 2015.
- Condos C, James A, Every P, Simpson T. Ten usability principles for the development of effective WAP and m-commerce services. Aslib Proc. 2002;54(6):345–55. https://doi.org/10.1108/00012530210452546
- Caldiera VRBG, Rombach HD. The goal question metric approach. In: Encyclopedia of software engineering. 1994; p. 528–32.
- Hussain A, Kutar M. Usability metric framework for mobile phone application. In: Proc. 10th Annu. PostGraduate Symp. 2009; p. 978–82.
- Harrison R, Flood D, Duce D. Usability of mobile applications: literature review and rationale for a new usability model. J Interact Sci. 2013;1(1):1. https://doi.org/10.1186/2194-0827-1-1
- Bertini E, Catarci T, Dix A, Gabrielli S, Kimani S, Santucci G. Appropriating heuristic evaluation for mobile computing. Int J Mob Hum Comput Interact. 2009;1(1):20–41. https://doi.org/10.4018/jmhci.2009010102
- Kaufman D, Roberts WD, Merrill J, Lai TY, Bakken S. Applying an evaluation framework for health information system design, development, and implementation. Nurs Res. 2006;55(Supplement 1):S37–42. https://doi.org/10.1097/00006199-200603001-00007
- van Gemert-Pijnen JEWC, Nijland N, van Limburg M, Ossebaard HC, M Kelders SM, Eysenbach G. A holistic framework to improve the uptake and impact of eHealth technologies. J Med Internet Res. 2011;13(4):e111. https://doi.org/10.2196/jmir.1672
- Halim MJ. The eHealth usability matrix: developing a usability evaluation framework for patient-facing ehealth technologies. University of Twente; 2019.
- Yen PY, Wantland D, Bakken S. Development of a Customizable Health IT Usability Evaluation Scale. AMIA Annu Symp Proc. 2010:917–21.
- Yen PY, Bakken S. Review of health information technology usability study methodologies. J Am Med Inform Assoc. 2012;19(3):413–22. https://doi.org/10.1136/amiajnl-2010-000020
- Cho H, Yen PY, Dowding D, Merrill JA, Schnall R. A multi-level usability evaluation of mobile health applications: a case study. J Biomed Inform. 2018;86:79–89. https://doi.org/10.1016/j.jbi.2018.08.012
- Wildenbos GA, Peute L, Jaspers M. Ageing barriers influencing mobile health usability for older adults: a literature based framework (MOLD-US). Int J Med Inf. 2018;114:66–75.
- Hussain A, Ferneley E. Usability metric for mobile application: a goal question metric (GQM) approach. In: Paper presented at the proceedings of the 10th international conference on information integration and web-based applications & services. 2008.
- Vollmer Dahlke D, Ory M. mHealth applications use and potential for older adults, overview of. Encyclopedia Geropsychology. 2015; p. 1–9.
- Zhang J, Walji MF. TURF: toward a unified framework of EHR usability. J Biomed Inform. 2011;44(6):1056–67. https://doi.org/10.1016/j.jbi.2011.08.005
- Kim S, Choudhury A. Comparison of older and younger adults’ attitudes toward the adoption and use of activity trackers. JMIR MHealth UHealth. 2020;8(10):e18312. https://doi.org/10.2196/18312
- Ahmad NA, Mat Ludin AF, Shahar S, Mohd Noah SA, Mohd Tohit N. Willingness, perceived barriers and motivators in adopting mobile applications for health-related interventions among older adults: a scoping review protocol. BMJ Open. 2020;10(3):e033870. https://doi.org/10.1136/bmjopen-2019-033870
- Saparamadu AADNS, Fernando P, Zeng P, Teo H, Goh A, Lee JMY. User-centered design process of an mHealth app for health professionals: case study. JMIR MHealth UHealth. 2021;9(3):e18079. https://doi.org/10.2196/18079
- Duque E, Fonseca G, Vieira H, Gontijo G, Ishitani L. A systematic literature review on user centered design and participatory design with older people. In: Proceedings of the 18th Brazilian symposium on human factors in computing systems. ACM; 2019.
- Helbostad JL, Vereijken B, Becker C, Todd C, Taraldsen K, Pijnappels M. Mobile health applications to promote active and healthy ageing. Sensors (Basel). 2017;17(3). https://doi.org/10.3390/s17030622
- Suastika K, Dwipayana P, Siswadi M, Tuty RA. Age is an important risk factor for type 2 diabetes mellitus and cardiovascular diseases. In: Glucose Tolerance. InTech; 2012.
- Saleh AM, Ismail RB. Usability evaluation frameworks of mobile application: a mini-systematic literature review. Global Summit on Education GSE. 2015.
- Liew MS, Zhang J, See J, Ong YL. Usability challenges for health and wellness mobile apps: mixed-methods study among mHealth experts and consumers. JMIR MHealth UHealth. 2019;7(1):e12160. https://doi.org/10.2196/12160
- Li C, Neugroschl J, Zhu CW, Aloysi A, Schimming CA, Cai D. Design considerations for mobile health applications targeting older adults. J Alzheimers Dis. 2021;79(1):1–8. https://doi.org/10.3233/JAD-200485
- Hussain A, Kutar M. Usability evaluation of SatNav application on mobile phone using mGQM. Int J Comp Inf Syst Ind Manag Appl. 2012;4:92–100.
- Ahmad N, Shoaib U, Prinetto P. Usability of online assistance from semiliterate users’ perspective. Int J Hum Comput Interact. 2015;31(1):55–64. https://doi.org/10.1080/10447318.2014.925772
Copyright Ownership: This is an open access article distributed in accordance with the Creative Commons Attribution Non Commercial (CC BY-NC 4.0) license, which permits others to distribute, adapt, enhance this work non-commercially, and license their derivative works on different terms, provided the original work is properly cited and the use is non-commercial. See: http://creativecommons.org/licenses/by-nc/4.0.